Table of Contents[Hide][Show]
- Reasons to Have a Tooth Pulled (Extracted)
- How much does a tooth extraction cost?
- How to Prepare for Tooth Extraction
- Anesthesia Options for Tooth Extraction
- Painkillers for Extraction Recovery
- Tooth Extraction Aftercare
- Recovery Time After Tooth Extraction
- Complications of Tooth Extraction
- When to Call Your Dentist
- Tooth Extraction vs. Root Canal vs. Fillings
- Orthodontics After Tooth Extraction
- Do you need a bone graft?
- FAQs
Tooth extraction is a dental procedure in which a tooth is pulled out of the socket in the bone where it rests.
Pulling teeth (extraction) may be necessary in cases of a deep cavity, wisdom teeth, broken teeth, and several other instances. However, some deep cavities can be restored — only unrestorable teeth would be candidates for extraction.
Depending on your exact issue, you may need a simple extraction or a surgical extraction. Surgical extractions have a longer healing process and come with a higher cost than simple tooth extractions.
Tooth extractions cost anywhere from $140-$450 per tooth. This cost is higher for surgical extractions. Other factors that influence cost include your location, experience of your dentist, and your specific needs.
IF YOU PURCHASE A PRODUCT USING A LINK BELOW, WE MAY RECEIVE A SMALL COMMISSION AT NO ADDITIONAL COST TO YOU. READ OUR AD POLICY HERE.
Simple vs. Surgical Tooth Extraction
There are two types of tooth extractions: simple tooth extraction and surgical tooth extraction.
Simple tooth extraction is a more routine procedure and only requires a local anesthetic.
Most general dentists offer simple tooth extractions. The healing time, pain management, and swelling will likely be more mild with a simple extraction.
Surgical tooth extraction requires a more invasive dental surgery procedure. Due to the more complex nature of surgical extraction, the recovery time, swelling, and pain may be a bit more extensive.
An oral surgeon could be needed for surgical extractions in some cases.
Your dentist determines whether or not you need a surgical or simple extraction using several factors:
- Visibility of the tooth
- Impaction of the tooth (usually, related to wisdom teeth)
- Hidden tooth root structure
Get Dr. B’s Dental Health Tips
You can’t be healthy without a healthy mouth. Sign up for my free newsletter and you’ll get my unconventional tips, starting with: If I had a cavity, here’s exactly what I’d do to reverse it.

Reasons to Have a Tooth Pulled (Extracted)
Reasons your dentist may suggest you have a tooth pulled include:
- Large cavities: Large areas of tooth decay can cause pulpitis, an inflammation and infection of the pulp (living tissue) inside your tooth. Pulpitis causes toothache and eventually progresses to irreversible pulpitis. If you have a large cavity that causes irreversible pulpitis, the tooth must be root canaled or extracted to prevent further complications.
- Wisdom teeth: Third molars (wisdom teeth) can grow in incorrectly, cause issues with crowding, develop cavities, and cause pain. Impacted wisdom teeth also pose risk of infection, inflammation, or gum irritation if not removed. Wisdom teeth removal is usually done between the ages of 17-25.
- Cracked/broken tooth: Depending on the level of damage, the dentist may recommend pulling the tooth instead of repairing it.
- Periodontal disease: In its more advanced stages, gum disease can loosen teeth within the mouth. These loose and weakened teeth will only continue to cause issues if not removed.
- Overcrowding: Removing a tooth can free up space for better orthodontic alignment. This may be necessary for orthodontic treatments, such as braces that shift teeth around inside the mouth.
- Overlap: A patient’s permanent teeth may start to come in before their “baby teeth” have fallen out, a condition known as hyperdontia. The dentist may remove the smaller teeth and make room for the permanent ones.
- Infection: In some cases, bad bacteria has spread into the tooth roots past what root canal therapy can treat.
- Compromised immunity: Patients with weakened immune systems (like from HIV/AIDS or chemotherapy) can have a harder time preventing tooth decay and infection, necessitating tooth extraction.
How much does a tooth extraction cost?
Tooth extraction costs $140-$450 per tooth in the United States.
Simple tooth extraction costs $187 per tooth on average. This would be a case where the tooth has grown above the gumline and has no complications.
Surgical tooth extraction costs $400 per tooth on average. Surgical extractions are usually performed on partially erupted or impacted teeth (like wisdom teeth).
Wisdom tooth extraction for all wisdom teeth costs $1,900 on average in the United States, including anesthesia, x-rays, and exams.
If you are planning for a dental implant after your tooth extraction, your dentist may recommend a bone graft be placed during the extraction procedure. Bone grafts cost anywhere from $200-$3,200, depending on the material you choose.
How to Prepare for Tooth Extraction
Your dentist will ask about all medications and supplements you take before the procedure. Your dentist needs to know if you currently take any of the below medications before your tooth extraction:
- Bisphosphonates
- Denosumab
- Anticoagulants (blood thinners), which may need to be discontinued before the extraction
- Steroids
- Immune-suppressing drugs
- Biological agents (like interleukins or vaccine therapy)
He or she also needs to know about any medical conditions you have, which may impact the chances of a successful extraction.
Conditions that have the most impact on tooth extraction outcomes include:
- Heart disease or defects (including hypertension, congenital heart defects, or damaged heart valves)
- Osteoporosis
- Bleeding conditions
- Diabetes
- Thyroid disease
- Liver disease
- Kidney disease
- Hormone-related conditions
- Artificial joints (like a hip replacement)
- Immune-suppressing conditions or circumstances (like HIV/AIDS or chemotherapy)
- History of bacterial endocarditis, an infection of the lining around the heart
The day of your dental procedure, keep the following in mind:
- If you will receive IV sedation (for moderate to deep sedation), be sure to wear a short-sleeved shirt so your veins are accessible.
- Don’t eat for 6-8 hours before the procedure if you are scheduled to get IV sedation.
- The day of the surgery, make sure you have a ride scheduled if you’ll be undergoing moderate or deep sedation.
- If you’ll be sedated, be sure that your ride is also ready to help with your post-care instructions until you’ve recovered from the effects of the anesthesia.
- Avoid smoking, which can greatly increase your risk for complications.
- During the week before the procedure, be sure to let your dentist know if you have had a cold or nausea and vomiting. You may need to reschedule or change anesthesia options.
Anesthesia Options for Tooth Extraction
Most simple tooth extractions don’t require anesthesia/sedation. Your dentist will inject a local anesthetic to the affected area to numb the tissue and reduce pain.
You may request the mild sedation option of nitrous oxide. Nitrous oxide, or “laughing gas,” will help keep your mind off the procedure but wears off within minutes so you can still drive yourself home.
For surgical extractions, anesthesia options include:
- Mild sedation: Nitrous oxide and/or a mild oral sedative. You can still drive home.
- Moderate sedation: Oral or IV Valium or another moderate sedative. You will need a ride home.
- Deep sedation: IV sedation administered by an anesthesiologist or dentist with special training, also known as general anesthesia. You will need a ride home.
Tooth Extraction Procedure: What to Expect
Before the Procedure
Before your tooth extraction, your dentist will perform a physical exam and take x-rays of the affected area.
He or she will also check for possible infections or cysts and observe your teeth’s relationship to your inferior alveolar nerve. This nerve essentially gives feeling to the entire bottom half of the mouth: jaw bone, lower lip, teeth, and chin.
Based on your medical history and x-ray, your dentist may prescribe antibiotics before the surgery. Factors include:
- The strength of your immune system
- The length of the surgery
- Infections or issues found in the x-ray
- Your medical history
Antibiotics for wisdom teeth removal or other tooth extractions may not be necessary, but no high-quality research has been done to know for sure. One report suggests antibiotics may actually increase the risk of some complications after tooth extractions.
For simple extractions, no sedation is usually necessary. If you need a surgical extraction, your dentist will talk to you about anesthesia options before your dental procedure.
During wisdom tooth extraction, your dentist will not need to plan for a dental implant later. However, if you have other teeth extracted that need an implant, a bone graft may need to be placed.
During the Procedure
You will feel pressure but should not experience pinching or pain during either a simple or surgical tooth extraction. If you experience any discomfort beyond the pressure your dentist describes, let them know right away.
The extraction process is slightly different between simple and surgical extractions.
Simple Tooth Extraction
During a simple extraction:
- Local anesthetic is injected into the affected area.
- Your dentist will loosen your tooth using an elevator instrument.
- He or she will pull out your tooth with forceps once it’s properly dislodged from the surrounding bone.
- Bone plates around the extraction site are squeezed together and filed to encourage healing. This is typically done only for wisdom tooth extraction, as an implant is not placed later.
- If you’re planning to get a dental implant after your extraction, a bone graft will be placed.
- The tooth socket is rinsed with a saline solution.
Surgical Tooth Extraction
During a surgical extraction:
- Local anesthetic is injected into the affected area.
- If IV sedation is being used, the IV will be inserted and the sedative will be administered.
- Your dentist will make a small incision into your gum line to access, loosen, and remove the tooth.
- The gums will be retracted to expose the underlying bone.
- Using a burr with a surgical motor, your dentist will remove some bone to expose the impacted tooth (if necessary).
- With an elevator instrument, your dentist will remove the exposed tooth.
- Your tooth socket will be rinsed with a saline solution.
- Your dentist will suture the extraction site closed.
- IV steroids may be administered to decrease post-procedure swelling.
After the Procedure
In the 60-90 minutes after your procedure, the local anesthesia will wear off. You may experience some discomfort and swelling (particularly after surgical extractions).
Most bleeding should subside within 4 hours after your extraction.
Your dentist or oral surgeon will send you home with a list of aftercare instructions. Be sure to follow these instructions for fast healing.
A gauze pad will be placed on the extraction site and your dentist will tell you to bite down on it. Bite down, but don’t chew on the gauze. Chewing can wiggle the blood clot and extend healing time.
Depending on your oral surgeon’s instructions, gauze should usually be removed 3-4 hours after tooth extraction. You may need to replace the gauze before that point if it becomes soaked with blood.
If you were given moderate or deep sedation, you may experience some side effects of anesthesia wearing off the 12 hours following your procedure. These most frequently include nausea and vomiting.
Painkillers for Extraction Recovery
Pain after tooth extractions can usually be managed with over-the-counter anti-inflammatory painkillers like ibuprofen (Motrin/Advil). In general, ibuprofen is more effective for dental pain relief than acetaminophen (Tylenol).
Avoid aspirin, as it can thin blood, increase, or continue bleeding.
Your doctor may also prescribe a short course of opioids after a surgical extraction. You’ll probably be advised to fill and pick up these prescriptions on your way home from the appointment. You should take your first dose of prescription pain medication before going to sleep.
Do not take opioids for longer than you absolutely need them, and take as small a dose as you can stand. You can use a pill cutter to take partial doses.
Be sure to dispose of any unused opioid pain medication as soon as possible. Be careful — not all medications should be flushed or thrown in a trash can.
What is the best painkiller for tooth extraction?
400-800 milligrams of ibuprofen is the best painkiller and dosage for tooth extraction. Many dentists recommend you take this dosage 3 times a day for 3 days after extraction, as it can also reduce your swelling.
However, this is considered a prescription dose and should not be taken unless your dentist prescribes it. Taking too high a dose of ibuprofen can thin the blood and promote bleeding in some cases.
Tooth Extraction Aftercare
Your dentist will update you with written aftercare instructions after your oral surgery. It’s important to follow them closely. This reduces your risk of complications like dry socket and infection.
For fast recovery after tooth extraction, follow these steps:
- Elevate your head: Lying flat can cause the blood vessels around the extraction site to throb and pulse, which can shorten healing time. Plan to keep your head elevated for 2-3 days after tooth extractions. Use a wedge pillow at night to keep your head elevated and a travel pillow during the day.
- Place a tea bag on the extraction site: Placing a damp, black tea bag (not herbal tea) on your wound can aid blood clotting and help your tooth extraction site heal faster.
- Ice the jaw: Use an ice pack on the side of your face as your tooth extraction at the first sign of swelling. Ice your jaw for 20 minutes on and 20 minutes off as often as you can for the first 36 hours after a surgical extraction like wisdom teeth removal. For extractions on both sides of your face, try a hands-free, wraparound ice pack.
- Avoid sucking or vigorous rinsing motions: Don’t do anything that can dislodge your blood clot, like drinking through a straw, spitting, or even passionate kissing. If you need to rinse your mouth, let the liquid roll around in your mouth, rather than physically swishing. Dislodging your blood clot early results in a painful condition known as dry socket.
- Use a salt water rinse: After 24 hours have passed, you can gently swish a warm salt water solution in your mouth to keep the extraction site clean and support fast healing. Place a teaspoon of salt (like Himalayan salt) at a time into warm water until it no longer dissolves, then allow the solution to rinse your mouth.
- Don’t smoke: Smoking will lengthen your recovery time considerably. Avoid smoking while you recover and use this time to kick the habit altogether if you can.
- Don’t touch the extraction site: Avoid poking the tooth socket with your tongue, finger, or any object while it heals.
- Eat soft foods for 2-3 days: Especially after a surgical extraction, focus on soft foods that won’t irritate your extraction site. Bone broth, coconut water, scrambled eggs, bananas, avocados, and applesauce are good foods for post-extraction healing. Avoid very sugary foods like ice cream or pudding, which can actually slow healing. Try the full shopping list from my free guide for tips after oral surgery.
How long after tooth extraction can I eat?
You can begin eating soft foods 4-6 hours after your tooth extraction.
When can I brush my teeth with toothpaste after tooth extraction?
You can start brushing your teeth with toothpaste 24 hours after tooth extraction. However, avoid brushing near the extraction site for at least 3 days.
You can also begin flossing normally 24 hours after your extraction while avoiding the extraction site.
Recovery Time After Tooth Extraction
Recovery time for a simple tooth extraction is about 2-3 days. You can usually return to normal activities after 2 days. The extraction site will usually heal completely in 14-21 days.
Recovery time for a surgical tooth extraction is generally 7-10 days. Expect to return to normal activities after 4-5 days. The extraction site takes about 4-6 months to heal completely.
How long does pain last after tooth extraction?
After simple tooth extractions, expect to feel mild pain or soreness for 1-2 days. Pain after surgical tooth extraction may last 3-7 days.
Complications of Tooth Extraction
Like all surgical procedures, tooth extraction does have a few possible complications. In general, most complications are associated with surgical and/or wisdom tooth extractions.
4.6% of patients experience complications after third molar (wisdom teeth) extractions.
Factors that increase your risk of tooth extraction complications include:
- Use of hormonal birth control
- Poor oral hygiene
- Wisdom teeth extraction, especially of bottom third molars
- Use of a surgical drill
- Inexperience of dental surgeon
- Age (the older the patient, the higher the risk)
- Presence of certain medical conditions in a patient’s medical history
- Distance of extracted tooth from the inferior alveolar nerve
- Existing infection before tooth extraction
Complications of tooth extraction may include:
- Dry socket: If a clot forms after tooth extraction but is dislodged too early — before day 4 of recovery — a dry socket is the result. This very painful condition is the most common complication of tooth extraction.
- Soreness in the jaw or mandibular joint: Many injections, long procedures, or lots of pressure will cause a bit of stiffness. This may be worse if you have pre-existing TMJ pain.
- Nearby damage: The teeth or any dental work could be damaged in a tooth extraction. In extreme cases, you may see cracked fillings or teeth.
- Infection: Postoperative infection is uncommon but can happen after tooth extraction (especially surgical extractions). Signs of infection after tooth extraction include fever, swelling longer than expected, tenderness of the jaw and/or infection site, and a foul taste or odor in the mouth.
- Sinus hole: A hole in the sinuses may open during extraction of a tooth in the upper back of the mouth. This will generally heal on its own after several weeks.
- Numb lips, tongue, or chin: An irritated inferior alveolar nerve can leave your lower lip, chin, or tongue still tingling or numb, called “paresthesia”. This may last 3-6 months in unusual cases. Rarely, this may be permanent.
- Leftover roots: your dentist may leave the tip of your tooth’s root behind if it poses a major risk to extract.
- Jaw weakness or fracture: This is uncommon and usually seen in older patients with complications. Likelihood of fracture increases with lower bone density or osteoporosis. The jaw may weaken over time without a dental implant.
- Orthodontic shift: Without a dental implant, an extraction site may allow teeth to shift. This can disrupt your bite and necessitate orthodontic treatment in the future.
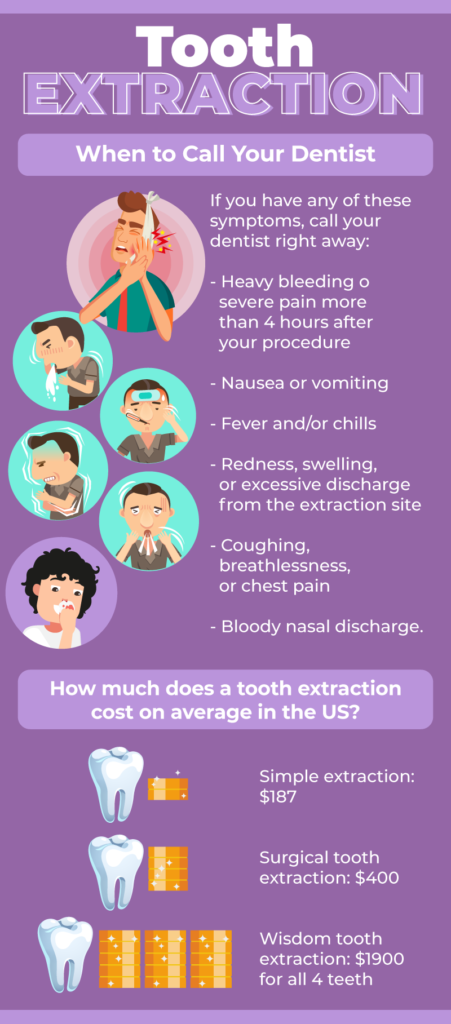
When to Call Your Dentist
Call your dentist if you experience:
- Heavy bleeding or severe pain more than 4 hours after your tooth extraction
- Nausea or vomiting
- Fever or chills
- Redness, swelling, or discharge from the extraction site
- Excessive bleeding from the tooth socket
- Coughing, breathlessness, or chest pain
- Bloody nasal discharge
Tooth Extraction vs. Root Canal vs. Fillings
When making a choice between a tooth extraction, root canal, fillings, or other restoration, make sure to talk to your dentist about the benefits and risks of each option.
For cavities that have not resulted in irreversible pulpitis, you may request a large dental filling and crown rather than an extraction.
Once irreversible pulpitis has set in, only a root canal or extraction with implant are viable options.
Your wisdom teeth may not need to be removed if they are not impacted and have enough space to come in. They can cause a temporary infection of the eruption site, called pericoronitis (the adult version of teething pain), but this may resolve in 2-3 weeks for healthy wisdom teeth.
Wisdom teeth extraction is generally not followed by a dental implant.
Many “natural health experts” encourage people to avoid root canals and always have teeth extracted instead. There are many supposed reasons for this, including the disproven focal infection theory, but much of it is based on flawed science.
When it comes to root canal vs. extraction, here’s what you need to know:
- The more teeth you have extracted (not root-canaled), the higher your risk for heart disease and cancer (regardless of your other risk factors).
- Root canals are more likely to fail if you have diabetes, high blood pressure, or your dentist doesn’t use proper sanitation methods.
- When you have a tooth extracted to get rid of a cavity, you’ll need a dental implant to fill the space, which comes with its own costs and other issues. A root canal requires a crown, but it will be less expensive than extraction and implant for most people over time.
- Root canals last longer, on average, than tooth extractions without additional work.
Orthodontics After Tooth Extraction
The American Academy of Periodontology has found that failure to address the space where your tooth once was can lead to shifting teeth, bite issues, and more.
Common orthodontic or restorative options after tooth extraction include:
- Dental implants: A dental implant fills the space left by an extracted tooth to allow for normal chewing and oral function. The process takes 3-12 months and costs $3,000-$4,500 per tooth on average.
- Bridges: A dental bridge consists of 1 or more dental implants anchored onto adjacent teeth with crowns. This can be a good option if more than one neighboring tooth was pulled. Bridges may cost anywhere between $2,000-$15,000.
- Braces: Orthodontic care after tooth extraction, like braces, may be required to prevent or correct shifting. Braces cost anywhere from $1,500-$10,000, depending on the type.
Do you need a bone graft?
If you’re going to get an implant, dental bridge, or denture after your extraction, talk to your surgeon about a bone graft during your tooth extraction.
When a tooth is removed, the alveolar bone it was attached to naturally tries to close in on itself. This can lead to bone loss, which can make procedures to replace that tooth more difficult (and expensive) down the road.
A bone graft is the process by which bone material (from your own bone, cow bone, or a synthetic bone graft material) is grafted into the existing alveolar bone. In the course of a few months, this allows for a strong base to grow that will support dental implants.
Research shows that doing a bone graft very soon after a tooth extraction greatly improved the quality of bone and alveolar ridge during healing. Bone grafting is a beneficial standard of care in nearly every case.
While a bone graft will increase the cost of your tooth extraction, it will be a better option financially (and physically) than waiting. Speak with your dentist or oral surgeon about this procedure when planning to have a tooth pulled.
Baby teeth should not require a bone graft after extraction.
FAQs
How many teeth can be extracted at the same time?
Technically, there is no limit to how many tooth can be extracted at the same time. Most dentists will recommend having all necessary extractions done at once to reduce overall healing time.
It’s a good idea to avoid bilateral extractions, or removing two opposing teeth at once, as this can interfere with chewing. However, wisdom teeth extraction is the exception to this rule.
Is tooth extraction painful?
Tooth extraction should not be painful. During the procedure, you should feel nothing more than pressure. Any pain should be immediately reported to the dentist performing the extraction.
If aftercare directions are followed closely, a tooth extraction should be mostly pain-free. In one study, patients receiving simple extractions said the procedure had very little effect on their quality of life.
Is bleeding normal after tooth extraction?
Some bleeding is normal for 4 hours after tooth extraction, especially surgical extraction of wisdom teeth. If you bleed excessively after 4 hours have passed, call your dentist.
What are the side effects of tooth extraction?
Short-term side effects of tooth extraction involve a small amount of pain and possibly a few missed workdays.
In the long-term, patients missing most or all of their teeth are at a greater risk of poor nutrition, plaque in the coronary artery, asthma, and diabetes. Periodontal disease leading to tooth loss can also affect other areas of health. However, implants can help with many of the alignment and jawbone issues caused by missing teeth.
What type of dental specialist performs tooth extractions?
An oral surgeon is a specialist that can perform extractions. All dentists are qualified to do tooth extractions, however.
Common reasons to seek treatment from an oral surgery include extraction of cracked teeth, extraction of impacted teeth, or referral from your general dentist. Oral surgeons are highly qualified to deal with a complex tooth extraction and any ensuing complications.
Residencies for oral surgeons require students to perform thousands of extractions before they even graduate. In fact, the average oral surgeon has studied for 12-14 years before certification. If it looks like your extraction could be difficult, an oral surgeon is a great route.
Is my tooth pain a dental emergency?
Your tooth pain may be a dental emergency if it is accompanied by excessive bleeding, fever, or swelling, which are signs of severe infection (like that caused by a tooth abscess). If you experience those symptoms or your pain is so severe that it disrupts normal activities like talking or eating, call your dentist right away.
However, most tooth pain (even pain that requires a tooth extraction) can be addressed by your dentist during normal business hours.
References
- Al‐Shammari, K. F., Al‐Khabbaz, A. K., Al‐Ansari, J. M., Neiva, R., & Wang, H. L. (2005). Risk indicators for tooth loss due to periodontal disease. Journal of periodontology, 76(11), 1910-1918. Abstract: https://pubmed.ncbi.nlm.nih.gov/16274310/
- Dodson, T. B. (1997). HIV status and the risk of post-extraction complications. Journal of dental research, 76(10), 1644-1652. Full Text: https://pubmed.ncbi.nlm.nih.gov/9326896/
- Hasegawa, T., Kawakita, A., Ueda, N., Funahara, R., Tachibana, A., Kobayashi, M., … & Yanamoto, S. (2017). A multicenter retrospective study of the risk factors associated with medication-related osteonecrosis of the jaw after tooth extraction in patients receiving oral bisphosphonate therapy: can primary wound closure and a drug holiday really prevent MRONJ?. Osteoporosis International, 28(8), 2465-2473. Abstract: https://pubmed.ncbi.nlm.nih.gov/28451732/
- do Nascimento Poubel, V. L., Silva, C. A. B., Mezzomo, L. A. M., Canto, G. D. L., & Rivero, E. R. C. (2018). The risk of osteonecrosis on alveolar healing after tooth extraction and systemic administration of antiresorptive drugs in rodents: a systematic review. Journal of Cranio-Maxillofacial Surgery, 46(2), 245-256. Abstract: https://pubmed.ncbi.nlm.nih.gov/29233703/
- Mingarro-de-León, A., Chaveli-López, B., & Gavaldá-Esteve, C. (2014). Dental management of patients receiving anticoagulant and/or antiplatelet treatment. Journal of clinical and experimental dentistry, 6(2), e155. Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4002346/
- Hayashi, M., Morimoto, Y., Iida, T., Tanaka, Y., & Sugiyama, S. (2018). Risk of delayed healing of tooth extraction wounds and osteonecrosis of the jaw among patients treated with potential immunosuppressive drugs: A retrospective cohort study. The Tohoku Journal of Experimental Medicine, 246(4), 257-264. Abstract: https://pubmed.ncbi.nlm.nih.gov/30568073/
- Lu, P., Gong, Y., Chen, Y., Cai, W., & Sheng, J. (2014). Safety analysis of tooth extraction in elderly patients with cardiovascular diseases. Medical science monitor: international medical journal of experimental and clinical research, 20, 782. Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4031223/
- Suda, K. J., Henschel, H., Patel, U., Fitzpatrick, M. A., & Evans, C. T. (2017, November). Use of antibiotic prophylaxis for tooth extractions, dental implants, and periodontal surgical procedures. In Open forum infectious diseases (Vol. 5, No. 1, p. ofx250). US: Oxford University Press. Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5757640/
- Marchionni, S., Toti, P., Barone, A., Covani, U., & Esposito, M. (2017). The effectiveness of systemic antibiotic prophylaxis in preventing local complications after tooth extraction. A systematic review. Eur J Oral Implantol, 10(2), 127-32. Abstract: https://europepmc.org/article/med/28555203
- Marghalani, A. (2014). Antibiotic prophylaxis reduces infectious complications but increases adverse effects after third-molar extraction in healthy patients. The Journal of the American Dental Association, 145(5), 476-478. Abstract: https://jada.ada.org/article/S0002-8177(14)60042-8/fulltext
- Dodson, T. B., & Susarla, S. M. (2010). Impacted wisdom teeth. BMJ clinical evidence, 2010. Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2907590/#BMJ_1302_I1205750731260
- Mamoun, J. (2017). Use of elevator instruments when luxating and extracting teeth in dentistry: clinical techniques. Journal of the Korean Association of Oral and Maxillofacial Surgeons, 43(3), 204-211. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5529197/
- Politis, C., Schoenaers, J., Jacobs, R., & Agbaje, J. O. (2016). Wound healing problems in the mouth. Frontiers in physiology, 7, 507. Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5089986/
- Sortino, F., & Cicciù, M. (2011). Strategies used to inhibit postoperative swelling following removal of impacted lower third molar. Dental research journal, 8(4), 162. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3221082/
- Stewart, M., Levey, E., & Nayyer, N. (2015). Salt water mouthwash post extraction reduced post operative complications. Evidence-based dentistry, 16(1), 27. Abstract: https://pubmed.ncbi.nlm.nih.gov/25909940/
- Younis, M. H. A., & Ra’ed, O. (2011). Dry socket: frequency, clinical picture, and risk factors in a palestinian dental teaching center. The open dentistry journal, 5, 7. Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3089956/
- Rakhshan, V. (2018). Common risk factors of dry socket (alveolitis osteitis) following dental extraction: A brief narrative review. Journal of stomatology, oral and maxillofacial surgery, 119(5), 407-411. Abstract: https://pubmed.ncbi.nlm.nih.gov/29723658/
- Rakhshan, V. (2015). Common risk factors for postoperative pain following the extraction of wisdom teeth. Journal of the Korean Association of Oral and Maxillofacial Surgeons, 41(2), 59-65. Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4411729/
- Momin, M., Albright, T., Leikin, J., Miloro, M., & Markiewicz, M. R. (2018). Patient morbidity among residents extracting third molars: does experience matter?. Oral surgery, oral medicine, oral pathology and oral radiology, 125(5), 415-422. Abstract: https://pubmed.ncbi.nlm.nih.gov/29397341/
- Bui, C. H., Seldin, E. B., & Dodson, T. B. (2003). Types, frequencies, and risk factors for complications after third molar extraction. Journal of Oral and Maxillofacial Surgery, 61(12), 1379-1389. Abstract: https://pubmed.ncbi.nlm.nih.gov/14663801/
- Friedman, J. W. (2007). The prophylactic extraction of third molars: a public health hazard. American journal of public health, 97(9), 1554-1559. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1963310/
- Vignoletti, F., Matesanz, P., Rodrigo, D., Figuero, E., Martin, C., & Sanz, M. (2012). Surgical protocols for ridge preservation after tooth extraction. A systematic review. Clinical Oral Implants Research, 23, 22-38. Abstract: https://pubmed.ncbi.nlm.nih.gov/22211304/
- Yeo, A. B., & Ong, M. M. (2004). Principles and implications of site preservation for alveolar ridge development. Singapore dental journal, 26(1), 15-20. Abstract: https://pubmed.ncbi.nlm.nih.gov/15736837/
- Oluwagbemigun, K., Dietrich, T., Pischon, N., Bergmann, M., & Boeing, H. (2015). Association between number of teeth and chronic systemic diseases: a cohort study followed for 13 years. PLoS One, 10(5), e0123879. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4422697/
- Virtanen, E., Söder, B., Andersson, L. C., Meurman, J. H., & Söder, P. Ö. (2014). History of dental infections associates with cancer in periodontally healthy subjects: a 24-year follow-up study from Sweden. Journal of Cancer, 5(2), 79. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3909762/
- Fouad, A. F., & Burleson, J. (2003). The effect of diabetes mellitus on endodontic treatment outcome: data from an electronic patient record. The Journal of the American Dental Association, 134(1), 43-51. Abstract: https://pubmed.ncbi.nlm.nih.gov/12555956/
- Debelian, G. J., Olsen, I., & Tronstad, L. (1995). Bacteremia in conjunction with endodontic therapy. Dental Traumatology, 11(3), 142-149. Abstract: https://pubmed.ncbi.nlm.nih.gov/7641631/
- Siqueira Jr, J. F. (2001). Aetiology of root canal treatment failure: why well‐treated teeth can fail. International endodontic journal, 34(1), 1-10. Full text: https://pdfs.semanticscholar.org/b103/6f37f3d451f884b787a667e4ba519a121b59.pdf
- Lekovic, V., Kenney, E. B., Weinlaender, M., Han, T., Klokkevold, P., Nedic, M., & Orsini, M. (1997). A bone regenerative approach to alveolar ridge maintenance following tooth extraction. Report of 10 cases. Journal of periodontology, 68(6), 563-570. Full text: https://www.researchgate.net/profile/Perry_Klokkevold/publication/14016455_A_Bone_Regenerative_Approach_to_Alveolar_Ridge_Maintenance_Following_Tooth_Extraction_Report_of_10_Cases/links/54f9ef150cf29a9fbd7c58d8.pdf
- Holm‐Pedersen, P., Lang, N. P., & Müller, F. (2007). What are the longevities of teeth and oral implants?. Clinical Oral Implants Research, 18, 15-19. Abstract: https://pubmed.ncbi.nlm.nih.gov/17594366/
- Adeyemo, W. L., Taiwo, O. A., Oderinu, O. H., Adeyemi, M. F., Ladeinde, A. L., & Ogunlewe, M. O. (2012). Oral health-related quality of life following non-surgical (routine) tooth extraction: A pilot study. Contemporary clinical dentistry, 3(4), 427. Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3636819/
- Felton, D. A. (2009). Edentulism and comorbid factors. Journal of Prosthodontics: Implant, Esthetic and Reconstructive Dentistry, 18(2), 88-96. Abstract: https://pubmed.ncbi.nlm.nih.gov/19254297/
- Meyer, M. S., Joshipura, K., Giovannucci, E., & Michaud, D. S. (2008). A review of the relationship between tooth loss, periodontal disease, and cancer. Cancer causes & control, 19(9), 895-907. Abstract: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2723958/
- Bell, R. B. (2016). Infinite cornucopia: the future of education and training in oral and maxillofacial surgery. Oral surgery, oral medicine, oral pathology and oral radiology, 121(5), 447-449. Abstract: https://www.oooojournal.net/article/S2212-4403(16)00078-X/abstract
- Roberts, G., Scully, C., & Shotts, R. (2000). Dental emergencies. Bmj, 321(7260), 559-562. Full Text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1071467/

 How to Find a Good Dentist: 7 Tips + 10 FAQs
How to Find a Good Dentist: 7 Tips + 10 FAQs