Table of Contents[Hide][Show]
Dry socket is a possible side effect of tooth extraction (including wisdom tooth removal) that occurs when the blood clot falls out of the extraction site too early.
Dry socket causes extreme pain in the extraction site that can radiate to the jaw and/or ear. It may also cause bad breath.
The highest risk for dry socket is between days 2-3 after a tooth extraction. After 4 days, the risk of dry socket has passed.
Dry socket pain can be treated at home and may resolve on its own within several days. Severe cases of dry socket, usually those that occur within the first day after tooth extraction, will need to be treated by your dentist.
IF YOU PURCHASE A PRODUCT USING A LINK BELOW, WE MAY RECEIVE A SMALL COMMISSION AT NO ADDITIONAL COST TO YOU. READ OUR AD POLICY HERE.
What is dry socket?
A dry socket is a painful condition when a blood clot that forms after a tooth extraction falls out too early. Losing the blood clot exposes the underlying bone and causes intense pain.
This usually happens after creating a sucking motion, like drinking through a straw, or through vigorous rinsing, like using mouthwash.
When a tooth is extracted from the jawbone, a blood clot forms in the empty hole left behind. Removal of the tooth leaves an empty hole in the jawbone that quickly fills with blood, forming blood clot within the first 24 hours.
The blood clot has two functions:
- To stop the extraction site from bleeding
- To stimulate bone healing
Remove that blood clot too soon — before the bone has healed — and you get a dry socket.
Sometimes, the blood clot is jostled free within the first few hours or days following extraction.
Without the blood clot present, the bone is fully exposed. This exposure causes intense pain that radiates up and down the face, as well as pain upon drinking cold water or breathing in cold air.
Get Dr. B’s Dental Health Tips
You can’t be healthy without a healthy mouth. Sign up for my free newsletter and you’ll get my unconventional tips, starting with: If I had a cavity, here’s exactly what I’d do to reverse it.

When can you get dry socket?
You can get a dry socket in the first 1-3 days after a tooth extraction or wisdom tooth surgery. Dry sockets are most common between days 2-3 after surgery.
When can you stop worrying about dry socket?
After the 4th day following extraction, you shouldn’t need to worry about getting a dry socket. By that point, the blood clot will have had enough time to establish itself.
What does dry socket look like?
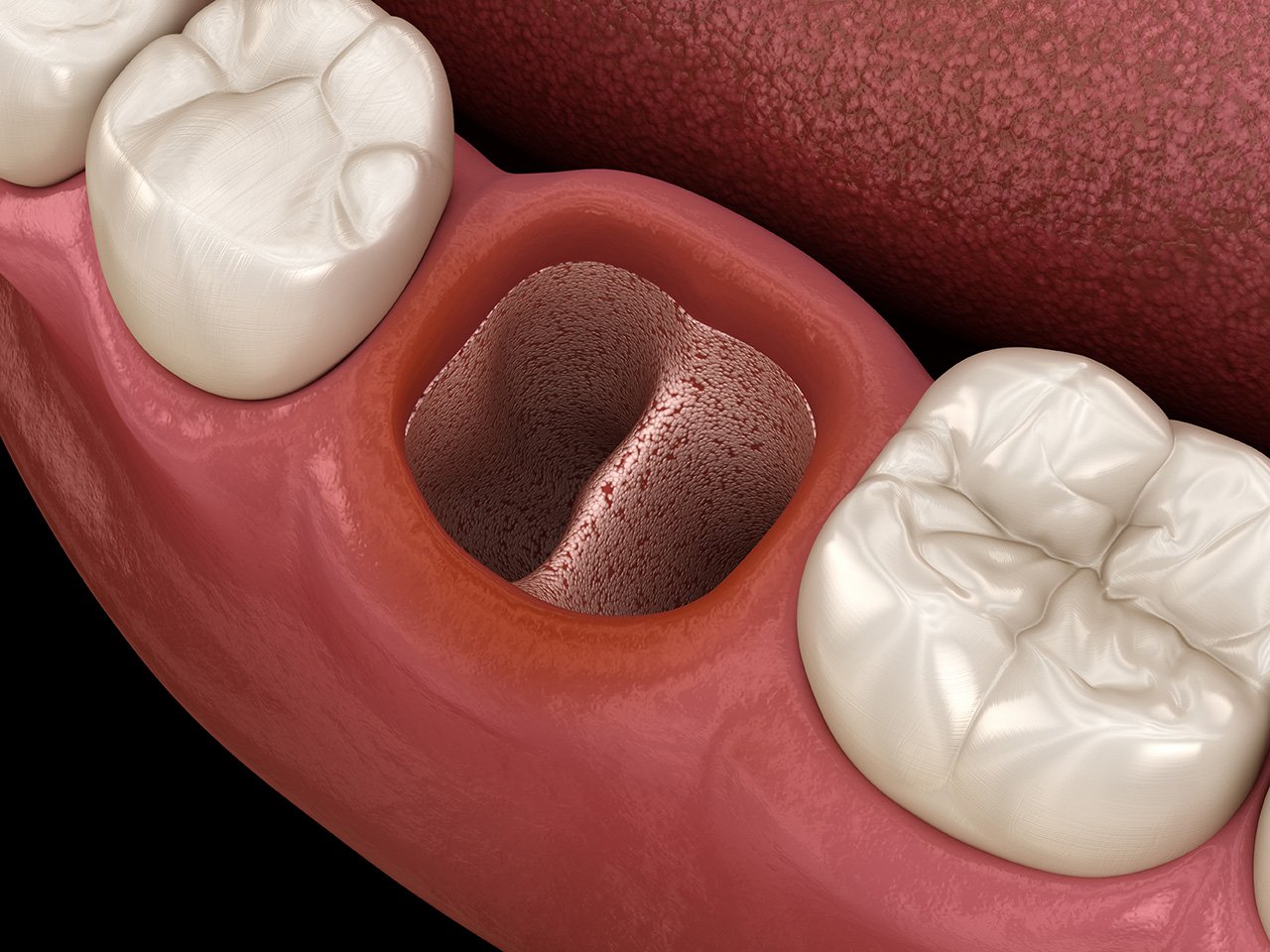
A dry socket looks like an empty tooth socket with a light color at the bottom of the extraction site.
The best way to spot a dry socket vs. normal tooth socket after extraction is that a dry socket appears as a hole with white-ish bone. There may be a thin tissue covering over the bone.
A normal socket, on the other hand, has a dark red blood clot on top of the bone.
Colors of material over the bone in a dry socket will differ between the types of dry socket you might have, ranging from grayish-green to yellow to a darker red.
Dry Socket Symptoms
Symptoms of dry socket include:
- Bleeding more than normal (if you develop a dry socket within 24 hours)
- Severe inflammatory, throbbing pain in your socket and radiating down into the bone or out to the ear
- Pain when the tooth is exposed to cool water or air
- Bad breath
- Bad taste in the mouth
- Headaches
- Dizziness
- Insomnia
- Infection (rare)
- Fever (rare)
In rare cases, dry socket leading to infection can end up causing trismus, also known as “lockjaw.” This would happen between 10-40 days following the loss of your blood clot.
What does dry socket feel like?
Dry socket pain feels like moderate-to-severe aching, sore pain that begins in the tooth socket and radiates out. The earlier the clot falls out, the more pain you’ll experience — and the more likely you’ll need a dentist’s help.
If you’re experiencing severe pain or bleeding 4 or more hours after a tooth has been extracted, contact your dentist immediately.
How do you know if you have dry socket?
The best way to know if you have a dry socket vs. normal tooth extraction pain is timing. Dry socket pain peaks 3-5 days after the extraction, while normal post-extraction pain peaks and wanes within the first day.
Dry Socket Treatment
Most cases of dry socket must be treated by your dentist. Your provider will decide how to treat dry socket based on the severity of your pain and the condition of your underlying bone.
Treatment options for dry socket include:
- Cleaning the tooth socket
- Medicated dressing with dry socket paste
- Bone grafting material
- Surgical foam
- Prescription pain relievers
1. Cleaning the tooth socket
Your dentist will remove food or other debris from above the exposed bone.
2. Medicated dressing with dry socket paste
Medicated dressings/gauze can offer pain relief by adding a pain relieving gel (medicated dry socket paste) to the underlying bone. Dry socket paste is 4% guaiacol and 4% eugenol in a base of petrolatum.
These dressings protect the extraction site from new food particles or debris.
Your dentist will instruct you as to how and when to remove the gauze. The medicated dressing may need to be changed several times while the extraction site heals. This is typically done every 24-48 hours for 3-6 days with a saltwater rinse or a prescription mouthwash.
3. Bone grafting material
By packing a dry socket with bone grafting material, your dentist can help the alveolar bone grow back more efficiently. This longer-term solution is most often used when a patient has thinner bone that will take longer to heal.
Bone grafting material is a more expensive solution than dry socket paste, which is why it’s used less often.
4. Surgical foam
Surgical foam may be placed in a dry socket to encourage wound healing and prevent excess bleeding from a dry socket. Like bone grafting material, surgical foam treatment is more expensive and used only in severe cases.
5. Prescription medications
Usually, over-the-counter painkillers are effective to relieve dry socket pain. However, your dentist may prescribe prescription painkillers for relief while your socket heals.
He or she may also prescribe antibiotics to prevent infection. If you already show signs of an infection from your open dry socket, this prescription can prevent more serious issues down the road (like lockjaw).
Home Care for Dry Socket Pain
Dry socket pain relief can typically be accomplished with over-the-counter pain medications, like ibuprofen (Advil) or acetaminophen (Tylenol). Other home remedies can help, too.
It’s important to note that the pain of a dry socket is not the same as pain in your teeth or gums. Analgesics (pain-relieving agents) like benzocaine (Orajel) are unlikely to provide much, if any, relief.
The best home remedies for dry socket pain include:
- Salt water rinse
- Honey
- Warm and/or cold compress
- Essential oils
- Tea bags
1. Salt water rinse
Gently swishing warm salt water can help to cleanse the exposed extraction site and reduce bacteria.
To make a salt water rinse for your dry socket:
- Pour about 8 ounces of warm water (not boiling).
- Add ½ a teaspoon of Celtic or Himalayan salt.
- Mix until the salt is dissolved.
- Very gently swish the rinse or just allow it to flood your mouth for about 30 seconds.
- Spit the mouth rinse into the sink.
Strong swishing motions can actually cause dry socket. They may also slow the healing process even after dry socket has been diagnosed.
For this reason, I recommend very gentle swishing or not swishing at all. Just letting the warm water flood the affected area and holding it in your mouth can be helpful.
2. Honey
Honey may reduce pain and inflammation caused by a dry socket.
Honey has been used as a treatment for wounds for hundreds of years. A 2014 study found that dressing a dry socket in honey helped with inflammation and reduced pain in patients. The treatment caused no side effects.
To use honey for dry socket:
- Put a ¼ teaspoon of honey on a sterile gauze.
- Place the gauze on the dry socket.
- Replace with fresh honey and sterile gauze every 3 hours.
3. Warm and/or cold compress
Press a cold towel or cold compress against your cheek near the dry socket to relieve inflammatory pain and swelling around the jaw bone. Do not hold ice directly against the skin; always use a towel or cloth between the ice and your skin.
Moist heat may be better for treating some tooth socket pain. Try warm heat after the first 24 hours after your tooth extraction, as long as the swelling has gone down.
4. Essential oils
Essential oils, including clove, oregano, and tea tree oil, may improve dry socket pain.
To apply essential oils for pain relief, mix them with a carrier oil, like coconut oil, before applying.
Don’t use them for longer than a few days. Essential oils have antibacterial properties that can kill good bacteria in the mouth and disrupt the oral microbiome if used extensively.
5. Tea bags
Green, black, or oolong tea bags can help reduce the pain and inflammation of a dry socket. Use a wet tea bag against the tooth socket for pain relief.
Be sure to use real tea from tea leaves, not herbal tea.
You may also put a slightly moist tea bag in a refrigerator first to use it as a cold compress.
Dry Socket Healing Time
Dry socket typically heals within 7-10 days. After this time, new tissue has been able to cover the visible bone and the wound has begun to heal.
For patients with thin alveolar bone, such as those with periodontal disease, healing may take longer.
How long does dry socket pain last?
Dry socket pain may 1-2 weeks to go away unless treated by a professional.
How To Prevent Dry Socket
You can prevent dry socket by following the instructions your dentist gives you following a tooth extraction (including wisdom tooth extraction). Your dentist may also employ several techniques that can help prevent dry socket.
To avoid dry socket for fast recovery after tooth extraction:
- Do not use straws
- Do not smoke cigarettes, vape pens, or marijuana
- Do not use any tobacco products
- Avoid vigorously swishing anything in your mouth
- Do not soak gauze pads in water before placing them on the extraction site
- Take antibiotics, if prescribed
- Avoid passionate kissing
- Do not drink carbonated and/or sugar beverages, like soda or lemonade
- Avoid sharp, spicy, or very hot foods (follow a soft foods diet for the 4 days after your oral surgery)
- Do not participate in strenuous exercise
- Try not to cough, sneeze, or spit
Talk to your dentist before your tooth extraction about these oral surgery techniques that may help prevent dry socket:
- Platelet-rich fibrin (PRF)
- Platelet-rich plasma (PRP)
- Prescription antibiotic mouthwash
- Medicated antibiotic dressing in gel foam
- Resorbable sutures
Causes & Risk Factors of Dry Socket
Dry socket is caused by dislodging the blood clot from a tooth extraction within the first 4 days after the procedure.
Certain risk factors increase your risk of dry socket, including:
- Female gender
- Age between 40-45
- Extraction of impacted wisdom teeth (third molars)
- Smoking or other tobacco use before or after tooth extraction
- Hormonal birth control pills
- Tissue trauma during tooth extraction
- Poor oral hygiene or oral health before extraction
- Underlying gum disease
- Dry sockets in the past
- Medical conditions that compromise immunity (like HIV/AIDS)
How common is dry socket?
Dry socket statistics vary by the type of tooth extraction and where your extraction site is.
- Dry sockets happen about 4% of the time across all types of tooth extractions.
- The extraction of a bottom tooth is 10 times more likely to result in a dry socket than a top tooth.
- Dry sockets occur after up to 25-45% of impacted wisdom teeth removals.
- Patients between 40-45 years old are most likely to develop a dry socket.
Types of Dry Sockets
There are several medical terms your dentist or oral surgeon may use to define your dry socket. The terms refer to different onset and symptoms.
In general, a dry socket is one condition with various complications. There are different terms that define the specifics of the “complications” of a dry socket.
You’ll notice the term “osteitis” used in several of the names listed below. This term refers to inflammation of the bone.
Alveolar Osteitis: This is the basic term for dry socket. It simply means inflammation of the bones that hold your teeth. Other terms for basic dry socket are:
- Localized osteitis
- Alveolitis
- Alveolitis sicca dolorosa
- Septic socket
- Necrotic socket
- Localized osteomyelitis of the mandible
- Fibrinolytic alveolitis
- Alveolitis simplex
A basic dry socket may leave bone exposed to the naked eye or look dark. It causes intense pain that doesn’t stop and may radiate throughout that side of the face. Fever and enlarged lymph nodes are rare but known symptoms of dry socket.
Superficial Alveolitis Marginal: SAM is classified by the covering of bone tissue in dry socket with inflamed tissue called a granuloma (inflamed grouping of tissue your body can’t get rid of). SAM makes it painful to chew.
Suppurative Alveolitis: This more serious issue is actually similar to dry socket but does not involve the clot falling out of your tooth’s socket. Instead, the blood clot gets inflamed from bone fragments or bone lesions called “osseous sequestrum.”
In suppurative alveolitis, the bone becomes inflamed because of the inflamed blood clot. Your oral surgeon would recognize this because the clot develops a membrane on top that turns grayish-green.
The pain of suppurative alveolitis is medium, as dry socket pain goes. You’re also more likely to get a fever with this form of dry socket.
FAQs
Why does a dry socket hurt so much?
Exposing the bone at the extraction site exposes the pain receptors in the jawbone to the outside world. Pain receptors in bones are some of the most alarmist of the nerve pain receptors.
This just means that they hurt. A lot.
Think of the blood clot as a scab on a deep cut on your skin. If the scab comes off too early, the area is exposed and can be extremely painful. It’s also more susceptible to infection.For these reasons, It’s imperative to keep the blood clot in the socket until the bone has a chance to fill the empty socket and heal. Without the blood clot, the socket will take longer to get better and will cause a lot of pain until the tooth extraction healing is complete.
Is dry socket dangerous?
It’s not a life-threatening condition, but a dry socket can cause severe pain and sometimes lead to infection.
Untreated, early dry socket might cause infections that cause an abscess or other infection-related symptoms, like fever.There are no known cases of death from dry socket or the subsequent infections.
Can a dry socket go away on its own?
Depending on when the clot comes out, some cases of dry socket may heal on their own. If you developed the condition on days 3 or 4 after tooth extraction, the pain probably won’t last for more than a week and will go away without treatment.
However, a clot falling out on the first or second day after your procedure might require more serious dry socket treatment.
Most cases of dry socket typically heal between 7-10 days after they happen, with untreated, severe dry socket causing potential pain for up to 2-3 weeks.
Can you get a dry socket with stitches?
Yes, you can get a dry socket with stitches. A blood clot can come out from a tooth socket between stitches. However, resorbable sutures may reduce the risk of developing a dry socket.
Can coughing cause dry socket?
Yes, coughing (or sneezing, or spitting) may lead to a dry socket. Anything that can dislodge a blood clot may lead to this tooth extraction complication.
References
- Singh, V., Pal, U. S., Singh, R., & Soni, N. (2014). Honey a sweet approach to alveolar osteitis: A study. National journal of maxillofacial surgery, 5(1), 31. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4178352/
- Ramos, E., Santamaría, J., Santamaría, G., Barbier, L., & Arteagoitia, I. (2016). Do systemic antibiotics prevent dry socket and infection after third molar extraction? A systematic review and meta-analysis. Oral surgery, oral medicine, oral pathology and oral radiology, 122(4), 403-425. Abstract: https://pubmed.ncbi.nlm.nih.gov/27499028/
- Sharma, A., Aggarwal, N., Rastogi, S., Choudhury, R., & Tripathi, S. (2017). Effectiveness of platelet-rich fibrin in the management of pain and delayed wound healing associated with established alveolar osteitis (dry socket). European journal of dentistry, 11(4), 508. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5727738/
- Rutkowski, J. L., Fennell, J. W., Kern, J. C., Madison, D. E., & Johnson, D. A. (2007). Inhibition of alveolar osteitis in mandibular tooth extraction sites using platelet-rich plasma. Journal of oral implantology, 33(3), 116-121. Abstract: https://pubmed.ncbi.nlm.nih.gov/17674676/
- Oringer, R. J. (2003). The combination of oral amoxicillin plus clavulanic acid and chlorhexidine rinses reduces the incidence of alveolar osteitis associated with the extraction of mandibular third molars. Journal of evidence based dental practice, 3(2), 77-81. Abstract: https://www.sciencedirect.com/science/article/abs/pii/S1532338203800234
- Fernandes, G. J., & Hatton, M. N. (2017). Prevention of Alveolar Osteitis: A Case Report and Review of Literature. Journal of the Michigan Dental Association, 82(1), 21-5. Full text: https://www.researchgate.net/profile/Gabriela_Fernandes/publication/321151119_Prevention_of_Alveolar_osteitis_case_report_and_review_of_literature_reprint/links/5a11d2b6a6fdccc2d79b64f8/Prevention-of-Alveolar-osteitis-case-report-and-review-of-literature-reprint.pdf
- Blum, I. R. (2002). Contemporary views on dry socket (alveolar osteitis): a clinical appraisal of standardization, aetiopathogenesis and management: a critical review. International journal of oral and maxillofacial surgery, 31(3), 309-317. Full text: https://www.researchgate.net/profile/Igor_Blum2/publication/11197833_Contemporary_views_on_dry_socket_alveolar_osteitis_A_clinical_appraisal_of_standardization_aetiopathogenesis_and_management_A_critical_review/links/59bedd67458515e9cfd22997/Contemporary-views-on-dry-socket-alveolar-osteitis-A-clinical-appraisal-of-standardization-aetiopathogenesis-and-management-A-critical-review.pdf
- Catellani, J. E., Harvey, S., Erickson, S. H., & Cherkin, D. (1980). Effect of oral contraceptive cycle on dry socket (localized alveolar osteitis). Journal of the American Dental Association (1939), 101(5), 777-780. Abstract: https://pubmed.ncbi.nlm.nih.gov/6935267/
- Cardoso, C. L., Rodrigues, M. T. V., Júnior, O. F., Garlet, G. P., & de Carvalho, P. S. P. (2010). Clinical concepts of dry socket. Journal of Oral and Maxillofacial Surgery, 68(8), 1922-1932. Full text: http://exodontia.info/files/J_Oral_Maxillofac_Surg_2010._Clinical_Concepts_of_Dry_Socket.pdf
- Hermesch, C. B., Hilton, T. J., Biesbrock, A. R., Baker, R. A., Cain-Hamlin, J., McClanahan, S. F., & Gerlach, R. W. (1998). Perioperative use of 0.12% chlorhexidine gluconate for the prevention of alveolar osteitis: efficacy and risk factor analysis. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontology, 85(4), 381-387. Abstract: https://pubmed.ncbi.nlm.nih.gov/9574945/

 ADA-Approved Denture Cleanser: Why do they contain this disturbing ingredient?
ADA-Approved Denture Cleanser: Why do they contain this disturbing ingredient?