Table of Contents[Hide][Show]
- What do wisdom teeth look like?
- Why do we have wisdom teeth?
- Symptoms of Erupting Wisdom Teeth
- Why Wisdom Teeth Cause Pain
- Wisdom Teeth Pain Relief
- Should you have your wisdom teeth removed?
- Antibiotics Before Wisdom Teeth Surgery
- Anesthesia Options for Wisdom Tooth Surgery
- Recovery After Wisdom Teeth Removal
- When to Call Your Dentist
- Complications After Wisdom Teeth Removal
- Cost of Wisdom Teeth Removal
- Prognosis and Long-Term Outlook
- FAQs
- Prevent Wisdom Teeth Removal
- Search the Functional Dentist Locator
- The Controversy of Wisdom Tooth Removal
About 10 million wisdom teeth are extracted from about 5 million patients every year in the United States.
Wisdom teeth usually come in during the late teens but can come in as early as 12 and as late as 26. They were dubbed “wisdom” teeth because you’re a little older and wiser when they come in as opposed to your other adult teeth.
Not all wisdom teeth should be removed, even if they initially cause pain.
Wisdom tooth pain can be treated effectively with ibuprofen and home remedies.
Wisdom teeth extraction costs between $75-$200 for simple extractions and $225-$600 for surgical extraction of impacted wisdom teeth. This is generally covered by dental insurance.
IF YOU PURCHASE A PRODUCT USING A LINK BELOW, WE MAY RECEIVE A SMALL COMMISSION AT NO ADDITIONAL COST TO YOU. READ OUR AD POLICY HERE.
What are wisdom teeth?
Wisdom teeth, or “third molars,” are the last teeth at the back of the top and bottom teeth arches. They come in between the ages of 12-26, though wisdom teeth most often erupt on their own between 17-21 years of age.
According to the AAOMS, 9 out of 10 people have at least one impacted wisdom tooth.
Around the age of 6, our adult teeth begin to come in, replacing the baby teeth we were born with. In most people, the central incisors are the first to emerge, followed by lateral incisors and first molars.
By age 13, most permanent teeth are in place — except for the wisdom teeth, that is. Wisdom teeth are the last adult teeth to erupt (completing the permanent dentition).
Wisdom teeth are completely unpredictable, in terms of both when they will arrive and whether they will erupt at all.
Some people don’t have any wisdom teeth, some have just 2 of 4, and others have a full set.
Unfortunately, if and when they do erupt on their own, wisdom teeth can bring a host of dental problems, including inflammation, swelling, and pain.
When our faces haven’t grown to their full potential, wisdom teeth simply don’t have enough room to emerge.
As a result, they can become impacted or infected. And, yes, they may need to be extracted.
Get Dr. B’s Dental Health Tips
You can’t be healthy without a healthy mouth. Sign up for my free newsletter and you’ll get my unconventional tips, starting with: If I had a cavity, here’s exactly what I’d do to reverse it.

What do wisdom teeth look like?
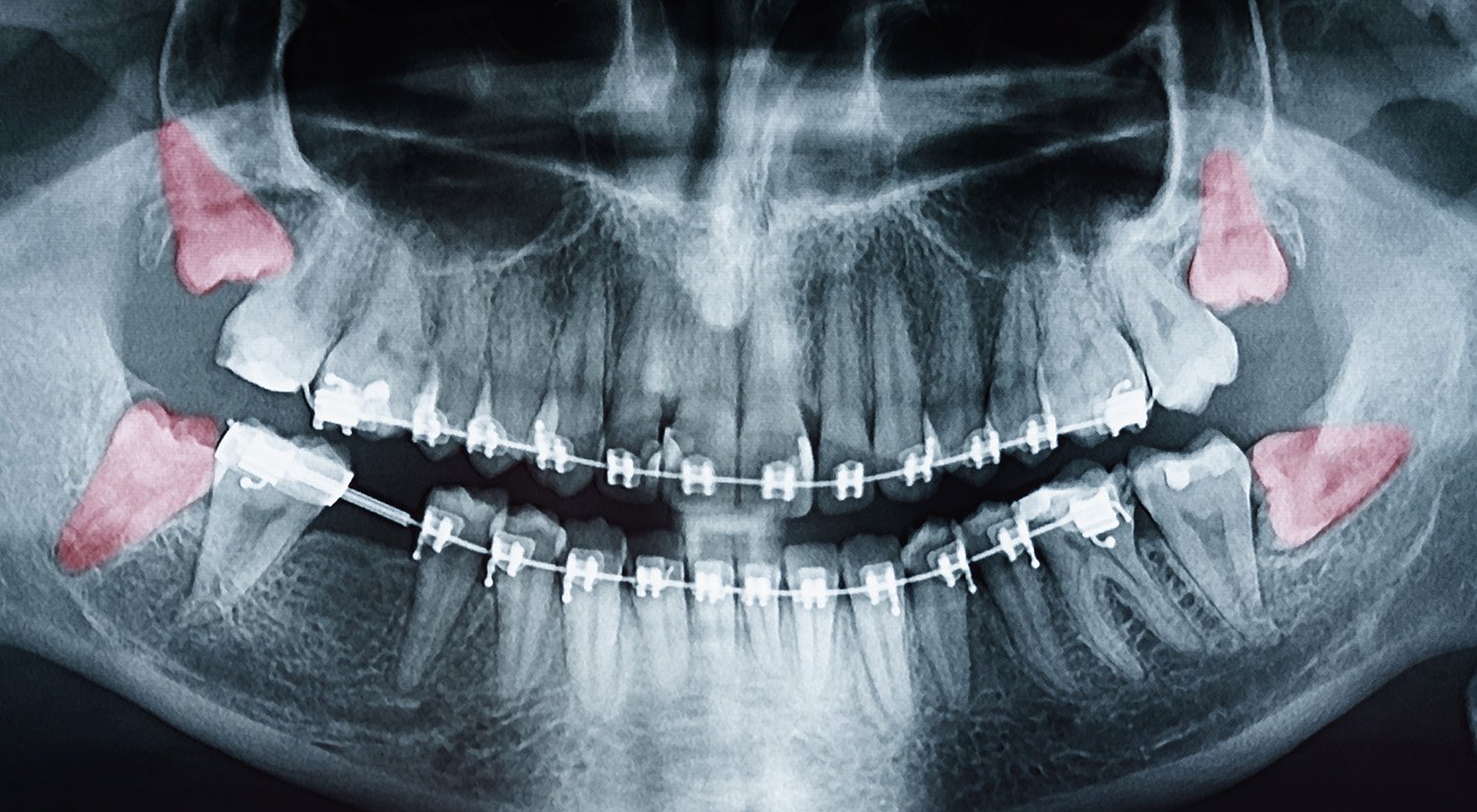
Wisdom teeth are a similar shape and size to your second molars, which generally come in between 12-13 years of age.
Why do we have wisdom teeth?
Wisdom teeth serve no purpose other than offering an extra set of molars for chewing food. Modern humans frequently have no space for their wisdom teeth due to a diet full of soft foods, deficiency of vitamin K2, and shorter breastfeeding times during infancy.
Third molars may have been useful for grinding plants during the Paleolithic era. The cellulose in plant cell walls is harder to digest than nutrients in meat, so it required extra pre-digestion in the form of chewing.
Because of changes in dietary patterns, wisdom teeth are widely considered “vestigial,” or a body part that no longer serves a significant purpose.
While most individuals in the 21st century don’t have enough room for their wisdom teeth, people in hunter-gatherer societies often did. Skulls of ancient humans have longer, wider jaws that were able to easily fit third molars.
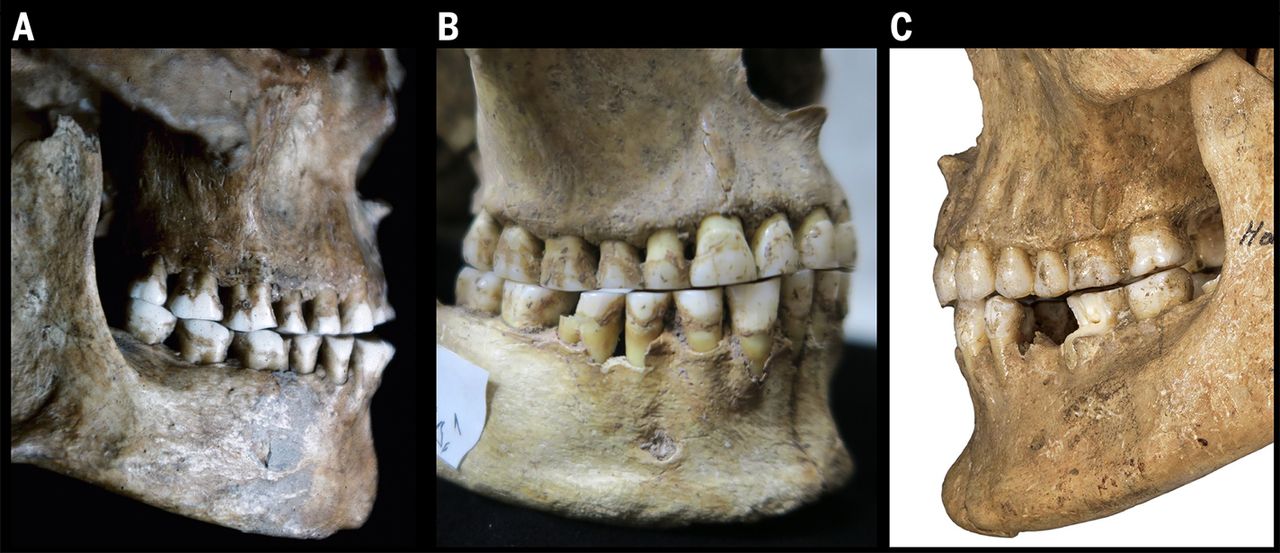
Unfortunately, we now have smaller jaws but the same number of teeth as our ancestors. Due mostly to our diets, we no longer have space for the last adult teeth to come in.
One reason for common modern-day problems with orthodontic growth is the lack of fresh, unprocessed foods in our diets compared to hunter-gatherer diets.
For instance, softer, processed foods require less chewing, which may impact the growth of the jaw. These were uncommon to find as staples in most diets before the Agricultural and Industrial Revolutions.
In addition, modern diets often contain too little vitamin K2, which may be responsible for the underdevelopment of our jaw.
Hunter-gatherers also practiced breastfeeding longer than modern human beings, which may also have better supported the full growth of the jaw.
Symptoms of Erupting Wisdom Teeth
A toothache is often the first sign of wisdom teeth coming in.
However, not all pain in the back of the mouth is a result of wisdom teeth. For instance, TMJ can cause similar symptoms to wisdom teeth.
Symptoms of erupting teeth include:
- Pressure or throbbing in your gums in the back of your mouth
- Swollen, red, or tender gums
- Visible cuts in your gums
- Persistent earache or headache
- A sinus infection that started at the same time as tooth pain
- Relief on vigorous brushing or rinsing in the area around your pain
- Swelling around your jaw
- Jaw stiffness
Earaches and headaches may occur when wisdom teeth erupt without enough room in the mouth. Pressure can build up around the surrounding teeth and tissues, causing significant pain in the mouth that is referred to other areas.
If your wisdom teeth have become damaged or infected, you may also experience bad breath, a bad taste, or problems fully opening your mouth.
A common misconception is that a change in the alignment of your teeth could be wisdom teeth causing crowding. However, there is no clinical evidence to support this popular theory.
The symptoms below suggest you are probably not experiencing erupting wisdom teeth but rather a cavity or other issue to discuss with your dentist:
- Tooth sensitivity to hot or cold
- Mild to sharp pain when you bite down
- A visible hole in your tooth
- Tooth discoloration
- Persistent toothache or sensitivity that lasts for at least a few minutes after exposure to hot, cold, or sweets
Why Wisdom Teeth Cause Pain
Generally, the pain from erupting wisdom teeth is due to a few causes:
- Pericoronitis: When wisdom teeth partially erupt, bacteria may enter the area and cause an infection, swelling, stiffness, and pain. This condition is called pericoronitis. It is essentially the adult version of teething and is the most common cause of wisdom teeth pain. If you don’t need your wisdom teeth extracted, this pain can be managed with pain relievers and a dental cleaning until it resolves on its own.
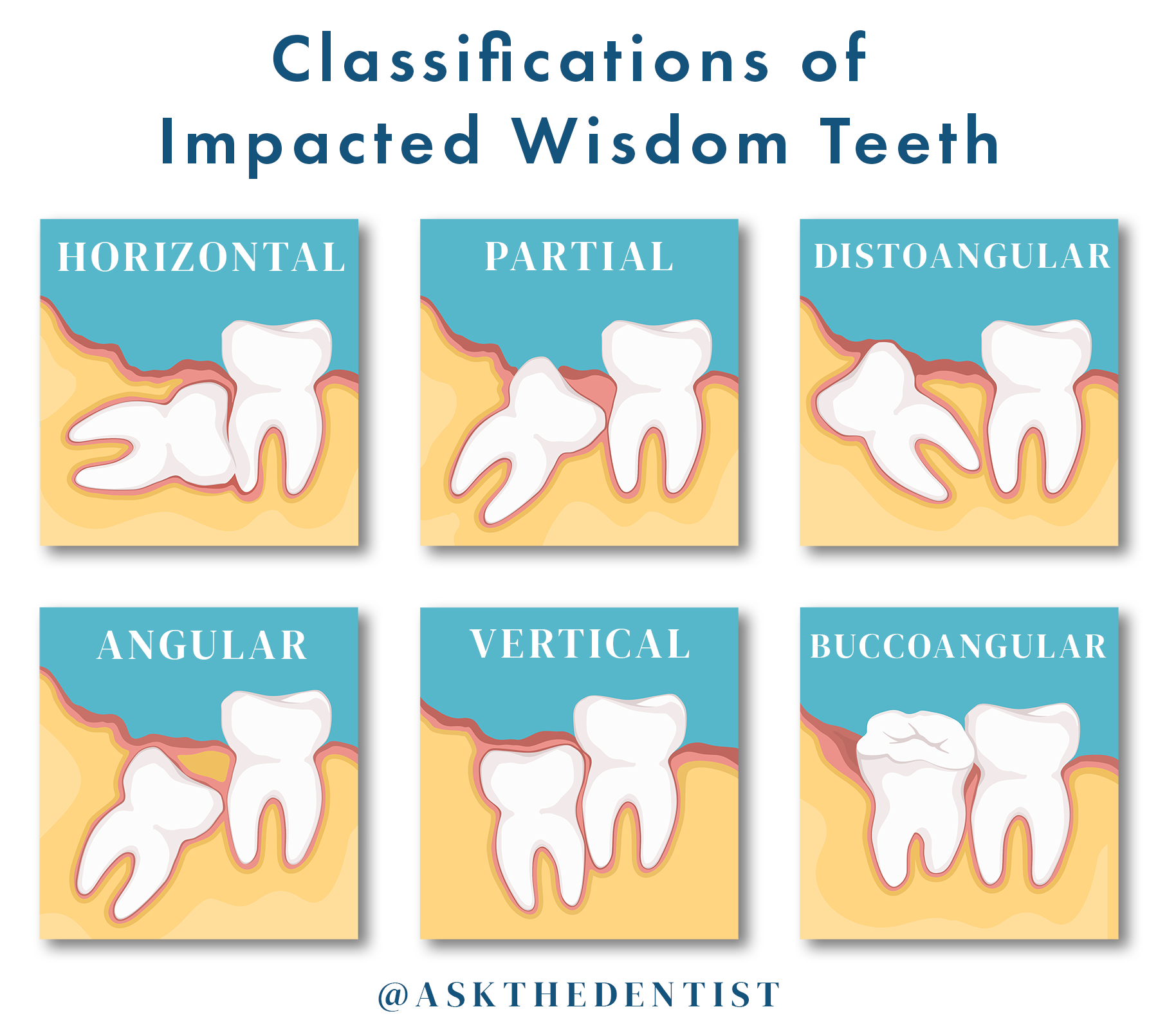
- Impaction: Often, a wisdom tooth tries to emerge without sufficient room to fully erupt. This can allow the tooth to attempt eruption at odd angles, pressing against other teeth. When these teeth begin to crowd, they cause soreness and generalized pain in the jaw near the impacted wisdom teeth. There are 6 basic classifications of wisdom tooth impaction.
- Cavities: Tooth decay, or “dental caries”, can form in the wisdom teeth and the adjacent second molars. Untreated tooth decay will eventually cause pain and sensitivity as inflammation and infection spread through the tooth.
- Cysts/tumors: A more serious cause of the pain can be the result of tumors or cysts forming around the impacted wisdom tooth. These lesions can lead to bone loss in the jawbone and destruction of other healthy teeth if not treated properly.
Wisdom Teeth Pain Relief
Pain relief for your growing wisdom teeth can be achieved with:
- Saltwater rinse: Use a super-saturated salt water rinse with Celtic salt or pink Himalayan salt 4-5 times daily to relieve gum inflammation from erupting wisdom teeth.
- Painkillers: Over-the-counter pain medication is generally enough to relieve pain caused by impacted wisdom teeth. Ibuprofen is best for toothache pain compared to acetaminophen (Tylenol). Your dentist may also prescribe a short supply (one week or less) of an opioid, such as hydrocodone (Vicodin) or Tylenol-3, for stronger pain relief.
- Benzocaine: This topical anesthetic gel can temporarily relieve pain in the gum and soft tissues of the mouth. Look for Orajel or Anbesol at your local drugstore or on Amazon.
- Clove oil: Clove essential oil may be as effective as benzocaine for pain relief in the mouth. Mix clove in a 1:1 ratio with a carrier oil like coconut oil and rub onto the affected gum area.
- Cold compress: For soreness of the jaw caused by tooth impaction, hold a cold compress or ice pack against the painful side of your face. An ice pack wrap can offer hands-free icing on both sides of your face — plus, it’s also helpful as you recover from surgery.
- Acupressure/acupuncture: Targeted acupressure and professional acupuncture are clinically proven to reduce dental pain. Check out this video for a demonstration of how to perform self-acupressure for different types of tooth pain.
- Antibiotics: Sometimes, your dentist may prescribe antibiotics if your wisdom teeth, second molars, or gums have become infected. In these cases, antibiotics may temporarily shrink the infection long enough to relieve pain. However, antibiotics are also frequently given to prevent dry socket. Unless you already have an infection, antibiotics are unlikely to relieve wisdom teeth pain.
How long does wisdom tooth growing pain last? The acute pain of wisdom teeth growing in should last for about 3-4 days and resolve on its own if the teeth are not impacted. Expect to feel soreness for 6-8 weeks and plan to regularly rinse with warm saltwater throughout that time.
If you choose not to extract impacted wisdom teeth, you could be in pain indefinitely, depending on the tooth position. However, not all impacted wisdom teeth cause pain.
Should you have your wisdom teeth removed?
Choosing to have wisdom teeth extracted is not always a straightforward decision, even if they are impacted. Not all wisdom teeth should be extracted, and you should consider the risks of wisdom teeth surgery versus the benefits of extraction.
You should have your wisdom teeth removed if:
- Your wisdom teeth are impacted and painful as they grow towards the second molars
- Your second or third molars (wisdom teeth) are infected or diseased
- The teeth are likely to cause orthodontic problems, such as crowding
- You’re at a high risk of developing tooth decay in the future
- You are at risk for periodontitis (gum disease) and related disorders (diabetes, heart disease, Alzheimer’s, etc.)
- You have recurring infections around or behind your back teeth
- You have a tumor or cyst near your wisdom tooth/teeth
- A wisdom tooth has become involved with the inferior alveolar nerve
You should probably not have your wisdom teeth removed if:
- Your jaw has the space to fit wisdom teeth without crowding
- You are in good health
- The teeth are not impacted
- You have TMJ and your wisdom teeth cause no symptoms
Pain is actually one of the worst indicators for a wisdom tooth removal. You should not have wisdom teeth removed just because they are causing pain. Your dentist can help you better determine if the pain is likely to pass or last.
If you are in the middle of orthodontic treatment, such as braces, you should delay wisdom teeth surgery, if possible, until your treatment is complete.
Talk to your dentist about their assessment of your wisdom teeth with an x-ray to determine if a wisdom tooth extraction is right for you.
Antibiotics Before Wisdom Teeth Surgery
For an infected wisdom tooth or as a preventative measure to protect against infection after your surgery, your dentist may prescribe any of the following antibiotics:
- Penicillin
- Amoxicillin
- Erythromycin
- Clindamycin
- Metronidazole
Prophylactic (preventative) antibiotics for wisdom tooth extraction are controversial, particularly as concerns about antibiotic resistance increase.
Some research suggests antibiotics may reduce infection around the surgical site and the risk of dry socket. Other research disagrees and claims prophylactic antibiotics do not significantly reduce the risk of either complication.
Anesthesia Options for Wisdom Tooth Surgery
For dental work, you typically have 3 levels of sedation to request: minimal, moderate, and deep sedation. There are multiple options at each level of sedation.
You and your oral surgeon can choose from various sedation options for wisdom tooth extraction:
- Local anesthesia (MINIMAL): Local anesthetic is injected at the surgical site to fully numb the inside and outside of the area around the affected tooth. It’s the same as you’d get for a filling. It does not actually result in sedation, just numbing. All wisdom teeth extractions utilize local anesthesia.
- Nitrous oxide (MINIMAL): This very safe, mild sedative helps you to feel calm and unconcerned during your dental procedure. It wears off quickly and you can expect to feel totally awake before going home. Nitrous oxide is only used for the extraction of non-impacted wisdom teeth.
- Oral sedatives (MODERATE): Valium (diazepam) is the most common oral sedative for moderate sedation during dental work. You’ll generally take one dose 45-60 minutes before your procedure. You might be groggy enough to fall asleep, but your dentist can easily wake you up.
- IV “conscious” sedation (MODERATE): You may opt for a similar sedative to Valium given intravenously. Similarly, you may sleep throughout some of the procedure but will wake easily.
- General anesthesia (DEEP): General anesthesia will cause you to fall completely to “sleep” and not able to be easily awakened. If you receive general anesthesia for wisdom teeth removal, your oral must have additional two-year certification or use an in-house anesthesiologist.
Minimal sedation is used for wisdom teeth extractions when the tooth is not impacted. Moderate or deep sedation may be utilized for impacted wisdom teeth removal.
Can I drive home after wisdom teeth removal? With only minimal sedation, you can drive home after your wisdom teeth removal surgery. If you receive moderate or deep sedation, you’ll need to arrange for someone else to drive you home.
Wisdom Tooth Removal Surgery: What to Expect
Before Surgery
Your dentist or oral surgeon will perform a full oral exam, including x-rays.
You’ll discuss several topics with your oral surgeon (or general dentist, if they’re performing the extraction) before surgery:
- Any medications you take
- Your medical history
- The type of anesthesia you need or want
- The exact date and time of your surgery
- Who will be driving you home from surgery, if more than local anesthetic will be used
During Surgery
Impacted wisdom tooth removal is an oral surgery that takes about 45 minutes from start to finish. It is an outpatient procedure, so you can go home after the extraction is complete.
Impacted wisdom teeth surgery, step-by-step:
- The dentist administers local anesthesia and sedation. (After this point, you’re not going to be aware of the procedure.)
- An incision will be made around the second molar and back through the top of your gums.
- The gums are retracted to expose the jawbone.
- The impacted tooth is exposed by removing some or all of the bone on the top and some of the bone along the sides using a burr with a surgical motor.
- It may be split into smaller pieces with the burr before extraction.
- The tooth is extracted using an elevator instrument.
- The tooth socket is rinsed with a saline solution.
- Sutures are placed to cover the tooth socket.
Simple tooth extraction, if your wisdom teeth are not impacted, take 20-30 minutes per tooth. This is an outpatient procedure that does not require moderate or deep sedation unless requested.
Most extracted wisdom teeth require surgical extractions (as described above). Simple wisdom tooth removal is the standard of care only if the teeth are already diseased — otherwise, they could remain in the mouth.
Simple wisdom teeth extraction, step-by-step:
- The dentist administers local anesthesia and sedation (if requested).
- The ligament fibers around the tooth are loosened with a periosteal elevator.
- The tooth is extracted with a dental elevator, using caution that the adjacent tooth is not injured.
- The bone plates are squeezed together and filed to facilitate healing.
- The tooth socket is rinsed with a saline solution.
After Surgery
You’ll notice when you wake up that your mouth is probably still numb. Local anesthesia will wear off 60-90 minutes after your procedure.
If you had impacted wisdom teeth removed, expect some blood in your mouth for the first 24 hours of recovery (especially for the first 4 hours).
Typically, you’ll be instructed to:
- Keep gauze over the extraction site and replace it if it gets soaked with blood for the first several hours after surgery.
- Fill prescriptions on your way home and take the first dose as soon as possible.
- Ice the side(s) of your face where teeth were extracted. Use an ice pack wrap for convenient, effective icing.
It’s normal to feel some nausea or even vomit within the first 10 hours of recovery. This typically happens because you swallowed blood or due to the sedatives wearing off.
Your oral surgeon will provide a list of what to do as you recover from wisdom tooth surgery.
In addition to gauze, icing, and medication guidelines, the instructions you get will probably discourage any physical activity or exertion for a few days.
Be sure to follow all instructions provided by your oral surgeon.
Recovery After Wisdom Teeth Removal
In many cases, you’ll be mostly recovered 3-4 days after wisdom teeth removal. It may take a week or more to heal after a complex surgery or if there were severe symptoms before your extraction.
Keep in mind that it takes 3-6 months for the tooth socket to heal completely. However, it is unlikely to cause any symptoms after 1-2 weeks have passed.
For fast wisdom tooth surgery recovery:
- Prevent dry socket, a painful complication of tooth extraction that occurs when you lose the blood clot too early from your healing tooth socket. Reduce your risk by avoiding straws, smoking, and vigorous rinsing for at least 3 days.
- Elevate your head, especially at night, for the first 72 hours to prevent throbbing pain. Use a wedge pillow or stack multiple pillows.
- Ice your cheeks for 36 hours to reduce inflammatory pain and swelling.
- Gently rinse your mouth with salt water a few times each day. This can reduce inflammation and prevent infection. Do not close your mouth or swish vigorously — it can cause a dry socket.
- Take over-the-counter anti-inflammatory medications through day 2 of recovery. Ibuprofen is the most effective pain reliever for wisdom teeth surgery recovery.
- Prevent dry mouth by nose breathing to cut down on your risk for postoperative infection. Use Biotene gel to keep the mouth moist if you can’t nose breathe.
- Massage your jaw (with caution) to relieve your masseter muscle that may have been exhausted after staying open during your surgery.
- Drink coconut water, which is loaded with important nutrients and may reduce inflammation. If the taste is off-putting, try my wisdom teeth pain relief smoothie.
- Sleep as much as you can.
- Avoid overusing medications by tapering off as soon as possible. You can use a pill cutter to divide doses in half, particularly for strong prescription opioids.
- Use moist heat to reduce bruising 36 hours after surgery. Some bruising through day 14 is normal, but it may go away after day 4 or anytime after.
Beginning on day 2, you should begin to gently brush and floss your teeth as normal. It’s vital to practice good dental hygiene for optimal oral health, as this reduces your risk of complications after surgery.
Your dentist will probably prescribe pain relief medication for recovery. Typically, these include hydrocodone (Vicodin) or Tylenol with codeine (Tylenol-3). Most people don’t need these after 3 days after wisdom tooth surgery.
What can you eat after wisdom teeth removal? For the first 24 hours after surgery, stick to liquids and very soft foods (mashed potatoes, etc.). On days 2 and 3, you can eat more foods to get enough calories but still avoid spicy, sharp, or hot foods.
Need more ideas? I designed a free guide with a comprehensive shopping list for easy-to-prepare foods you can eat after oral surgery.
Many dentists use dissolvable stitches. However, if your stitches must be removed manually, you’ll need to go back to your oral surgeon about 1 week after surgery.
When to Call Your Dentist
Call your dentist right away if you have any of these symptoms after wisdom teeth removal:
- Excessive bleeding past 4 hours after your surgery
- Throbbing pain that won’t go away
- Oozing pus
- Swelling that increases rather than going down
- Fever/chills
- Pain that spikes 48 hours after the extraction
- Nausea or vomiting after 10 hours post-op
- Vomiting significant amounts of blood (a little blood is normal)
- Coughing
- Chest pain
- Shortness of breath
- Difficulty swallowing or breathing
- Blood or pus from your nose
Complications After Wisdom Teeth Removal
In 1.2%-4.3% of cases, patients will experience complications after wisdom teeth removal.
Potential complications of wisdom tooth removal include:
- Dry socket: This painful condition happens after the blood clot is lost too early from the tooth socket. Generally, the risk of dry socket is highest on days 2-3 after surgery and is mostly gone after day 4. PRP (platelet-rich plasma) or PRF (platelet-rich fibrin) during surgery may reduce this risk. Dry socket is referred to in medical literature as alveolar osteitis.
- Paresthesia: If your inferior alveolar nerve is damaged during surgery, you may experience temporary or permanent numbness in the lips and tongue. This condition is called paresthesia.
- Infection: The wound may become infected after wisdom teeth extraction. A comprehensive study found that postoperative infection occurred in 0.8% of patients.
- Bleeding: Excessive bleeding that lasts beyond 10 hours can occur in some cases. On average, this may be the most common complication of having wisdom teeth removed. It occurred in 0.9% of patients in the study mentioned above.
Factors that increase your risk of complications include:
- Immunodeficiency (such as HIV/AIDS or autoimmune disease)
- Diabetes
- Heart disease
- Older age
- Certain medications, including corticosteroids, blood thinners, and birth control pills
- Pre-existing infection
- Periodontitis (gum disease)
- Poor dental hygiene
- An exceptionally difficult extraction
- Poor irrigation of the tooth socket
Cost of Wisdom Teeth Removal
Wisdom tooth removal costs $75-$200 per tooth for simple extractions and $240-$600 per tooth for surgical extractions. This may not include certain types of anesthesia, which could cost extra.
Most dental insurance plans cover wisdom teeth surgery at 80%. They frequently have a cap of $1,500 or less per year, so extraction of 4 impacted wisdom teeth is likely to max out your benefits for that calendar year.
Prognosis and Long-Term Outlook
Wisdom tooth removal surgery is a common, relatively safe procedure. While there are risks to any medical procedure or surgery, serious complications (like paresthesia) are very rare.
After wisdom tooth removal and recovery, you can go on as usual. Most of the time, this surgery requires little-to-no follow-up, especially if you are young and healthy.
If you choose not to have wisdom teeth removed because they cause no lasting symptoms, you may be at a higher risk of gum disease and cavities in the back of your mouth. Impacted wisdom teeth, even with no pain, are more likely to become infected.
Signs of infection include redness, swelling, pain, and bad breath (halitosis).
Be sure to keep up with your 6-month cleanings so your dentist can spot any problems that arise.
FAQs
What does Weston A. Price’s research tell us about why most people don’t have room for wisdom teeth?
Weston A. Price was a maverick of a dentist who, in 1939, published a fascinating report of how adjusting to a modern diet may actually shorten jaw growth. This gives further evidence that modern diets are a major reason industrialized people frequently have smaller jaws than people in hunter-gatherer societies.
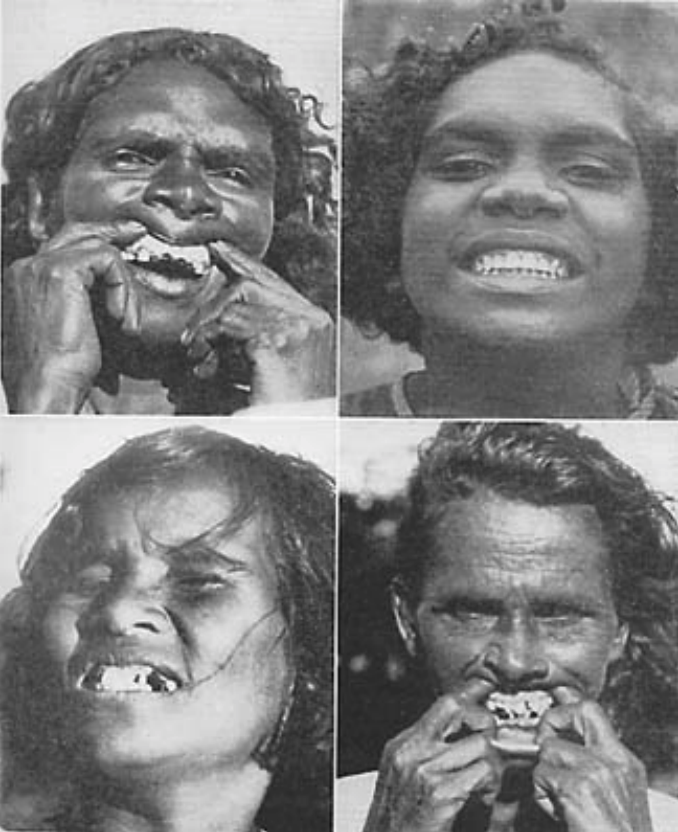
In the image above, Dr. Price compared images of Aboriginal women on traditional hunter-gatherer diets (top right) to those on a modernized, more processed diet.
The orthodontic growth of the jaws was dramatically limited in those with modern diets. Modern diets also led to alarmingly higher rates of cavities. Price saw the same phenomenon over and over in each primitive vs. modern society comparison he conducted.
Theories for the specifics of why this happened are primarily focused on the presence of vitamin K2 and the absence of processed sugars and carbohydrates.
If I’m not in pain, does that mean I shouldn’t have my wisdom teeth extracted?
Pain isn’t a great diagnostic tool for wisdom tooth extraction. Not everyone experiences wisdom tooth pain, but your dentist can tell you if you’re at risk of long-term problems by doing a full exam and x-ray.
Only one of my wisdom teeth hurt. Is that normal?
Not all wisdom teeth come in at the same time. Your wisdom teeth may not come in at the same time as your sister’s or your best friend’s did. All four of yours may not come in at once, either.
One tooth could be impacted in the gum tissue while three others may emerge with no problem. Two may come in at once and the other two might take another year or two. Dental x-rays and regular exams are the best way to stay aware of the progress, or lack thereof, of wisdom tooth eruption.
Is wisdom teeth surgery scary?
Having your wisdom teeth surgically removed can be daunting. However, this procedure does not have to be scary. Prepare for some pain and soreness during recovery. But keep in mind that, for painful, impacted wisdom teeth, the pain after your surgery is often more bearable than the pain that sent you to the dentist in the first place!
Does everyone have wisdom teeth?
No, not everyone has wisdom teeth. It’s not uncommon to have two or even zero wisdom teeth from birth. Your dentist can tell you if you have wisdom teeth by looking at an x-ray of your mouth.
Can wisdom tooth surgery cause a thinning of the face?
Yes, it’s possible that removal of your wisdom teeth may cause a minor thinning of your face shape.
Prevent Wisdom Teeth Removal
There’s not much you can do about an impacted wisdom tooth to make it more or less likely to cause problems. Good oral health is a great start, but you have no power over how your teeth are positioned.
But with very early intervention, you may be able to prevent the need for wisdom tooth removal by supporting the proper growth of the jaw bone.
I mean very early intervention — before pregnancy, if possible!
Follow these steps to support proper jaw growth during development:
- Supplement with and eat plenty of vitamin K2 during pregnancy and during childhood. The third trimester of pregnancy is most vital, as those 13 weeks are when the bottom of the face is formed in the womb — including the jaw — requiring the most vitamin K2 to that point. Give your child a kid’s cod liver oil once a day and eat grass-fed animal products whenever you can. To learn more about how K2 supports orthodontic growth, check out Vitamin K2 and the Calcium Paradox.
- Prevent mouth breathing, especially during childhood. Mouth breathing and/or sleep-disordered breathing may cause stunted orthodontic growth. Older children and teens can mouth tape at night, but mouth breathing and sleep-disordered breathing in babies and toddlers are more difficult to address.
- Get an orthodontic assessment for your child between 2-5 years of age. This is earlier than many traditional orthodontists recommend. However, if you address any orthodontic growth problems by the age of 5, your orthodontist can recommend palatal expanders and support the full growth of the jaw. If you wait for braces after the age of 10, the jaw has already done a lot of its growing. Search for an orthodontist who practices “Orthotropics” in our database.
Search the Functional Dentist Locator
Our database of functional providers includes dentists, hygienists, and myofunctional therapists, in over 50 areas around the world and growing.[/callout-quiz]The Controversy of Wisdom Tooth Removal
Until the early 2000s, almost all impacted wisdom teeth — and some healthy, non-impacted wisdom teeth — were extracted as a prophylactic, or preventative, measure.
The common thought process was that extracting most or all wisdom teeth would prevent future issues those teeth would otherwise create, like:
- Crowding and orthodontic problems
- Gum disease (periodontitis)
- Cavities (in the wisdom teeth or adjacent second molars, known as “distal cervical caries”)
- Dental surgery in aging patients, which carries a higher rate of failure
But in 2000, Great Britain’s National Health Service (NHS) issued guidelines stating that preventative removal of impacted wisdom teeth “should be discontinued”. They based this on 1997 guidelines from the Royal College of Surgeons.
A 2007 report on preventative extraction of wisdom teeth called the phenomenon “a public health hazard”. Dentist Jay Friedman, DDS explained in the report that around 1% of patients develop a lifelong condition called paresthesia after the removal of wisdom teeth.
According to his calculations, 9 million lost days of work and about $2.2 billion every year could be saved.
Friedman also discussed “myths” about the potential dangers of leaving asymptomatic wisdom teeth alone. For instance, he postulates that about 12% of impacted wisdom teeth will cause problems in nearby teeth or gums if not extracted.
As he points out, that rate is similar to that of infections of the gallbladder and appendix — but those procedures are not recommended as a standard of care.
The American Public Health Association issued a statement in 2008 affirming this position. They advise that wisdom teeth only be removed if there is “evidence of diagnosed pathology or demonstrable need.”
In 2016, the American Association of Oral and Maxillofacial Surgeons also recommended that healthy wisdom teeth not be extracted unless the surgeon thinks there is a high risk of future issues. Their public statement was supported by 11 similar organizations around the world.
More recently, other clinicians and organizations have spoken out about concerns based on these guidelines. Friedman’s popular “12%” figure may not be accurate after all.
A 2014 review suggests that 64% percent of patients who do not have impacted wisdom teeth extracted will need them extracted within 18 years.
Oral surgeon Louis W. McArdle, BDS, MSc, FDS wrote a 2019 paper about the increasing prevalence of distal cervical cavities (cavities in the second molar) as a complication of impacted wisdom teeth.
As a general dentist who has performed many third molar extractions over 35+ years, I recommend all partially or fully impacted wisdom teeth be removed. If the tooth is impacted, it will — not might, in my experience — cause issues later in life.
These extractions have a much higher chance of complications in elderly or immunocompromised patients. That’s why I don’t recommend my own patients keep impacted wisdom teeth, even in the absence of pain.
Ultimately, wisdom teeth removal is a decision you need to make with the input of your dentist. Whatever you decide, you can rest assured that millions of people are with you!
References
- Bailey E, Kashbour W, Shah N, Worthington HV, Renton TF, Coulthard P. Surgical techniques for the removal of mandibular wisdom teeth. Cochrane Database of Systematic Reviews 2020, Issue 7. Abstract: https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD004345.pub3/full
- Blasi, D. E., Moran, S., Moisik, S. R., Widmer, P., Dediu, D., & Bickel, B. (2019). Human sound systems are shaped by post-Neolithic changes in bite configuration. Science, 363(6432). Full text: https://science.sciencemag.org/content/363/6432/eaav3218
- von Cramon-Taubadel, N. (2011). Global human mandibular variation reflects differences in agricultural and hunter-gatherer subsistence strategies. Proceedings of the National Academy of Sciences, 108(49), 19546-19551. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3241821/
- Price, W. A., & Nguyen, T. (2016). Nutrition and physical degeneration: a comparison of primitive and modern diets and their effects. EnCognitive. Com. Full text: https://healthwyze.org/archive/nutrition_and_physical_degeneration_doctor_weston_a_price.pdf
- Falci, S. G. M., De Castro, C. R., Santos, R. C., de Souza Lima, L. D., Ramos-Jorge, M. L., Botelho, A. M., & Dos Santos, C. R. R. (2012). Association between the presence of a partially erupted mandibular third molar and the existence of caries in the distal of the second molars. International Journal of oral and maxillofacial surgery, 41(10), 1270-1274. Abstract: https://pubmed.ncbi.nlm.nih.gov/22464852/
- Obiechina, A. E., Arotiba, J. T., & Fasola, A. O. (2001). Third molar impaction: evaluation of the symptoms and pattern of impaction of mandibular third molar teeth in Nigerians. TROPICAL DENTAL JOURNAL, 22-25. Abstract: https://pubmed.ncbi.nlm.nih.gov/11484653/
- Bailey, E., Worthington, H. V., van Wijk, A., Yates, J. M., Coulthard, P., & Afzal, Z. (2013). Ibuprofen and/or paracetamol (acetaminophen) for pain relief after surgical removal of lower wisdom teeth. Cochrane Database of Systematic Reviews, (12). Full text: https://www.cochranelibrary.com/cdsr/doi/10.1002/14651858.CD004624.pub2/full
- Hersh, E. V., Ciancio, S. G., Kuperstein, A. S., Stoopler, E. T., Moore, P. A., Boynes, S. G., … & Shibly, O. (2013). An evaluation of 10 percent and 20 percent benzocaine gels in patients with acute toothaches: efficacy, tolerability and compliance with label dose administration directions. The Journal of the American Dental Association, 144(5), 517-526. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3844156/
- Alqareer, A., Alyahya, A., & Andersson, L. (2006). The effect of clove and benzocaine versus placebo as topical anesthetics. Journal of dentistry, 34(10), 747-750. Abstract: https://pubmed.ncbi.nlm.nih.gov/16530911/
- Naik, P. N., Kiran, R. A., Yalamanchal, S., Kumar, V. A., Goli, S., & Vashist, N. (2014). Acupuncture: an alternative therapy in dentistry and its possible applications. Medical acupuncture, 26(6), 308-314. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4270142/
- Renton, T., & Wilson, N. H. (2016). Problems with erupting wisdom teeth: signs, symptoms, and management. British Journal of General Practice, 66(649), e606-e608. Ful text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4979926/
- Halpern, L. R., & Dodson, T. B. (2007). Does prophylactic administration of systemic antibiotics prevent postoperative inflammatory complications after third molar surgery?. Journal of Oral and Maxillofacial Surgery, 65(2), 177-185. Abstract: https://pubmed.ncbi.nlm.nih.gov/17236918/
- Ren, Y. F., & Malmstrom, H. S. (2007). Effectiveness of antibiotic prophylaxis in third molar surgery: a meta-analysis of randomized controlled clinical trials. Journal of oral and maxillofacial surgery, 65(10), 1909-1921. Full tet: https://www.researchgate.net/profile/Yanfang_Ren/publication/5957787_Effectiveness_of_Antibiotic_Prophylaxis_in_Third_Molar_Surgery_A_Meta-Analysis_of_Randomized_Controlled_Clinical_Trials/links/59fc5d53a6fdcca1f294ee19/Effectiveness-of-Antibiotic-Prophylaxis-in-Third-Molar-Surgery-A-Meta-Analysis-of-Randomized-Controlled-Clinical-Trials.pdf
- Blum, I. R. (2002). Contemporary views on dry socket (alveolar osteitis): a clinical appraisal of standardization, aetiopathogenesis and management: a critical review. International Journal of oral and maxillofacial surgery, 31(3), 309-317. Full text: https://www.researchgate.net/profile/Igor_Blum2/publication/11197833_Contemporary_views_on_dry_socket_alveolar_osteitis_A_clinical_appraisal_of_standardization_aetiopathogenesis_and_management_A_critical_review/links/59bedd67458515e9cfd22997/Contemporary-views-on-dry-socket-alveolar-osteitis-A-clinical-appraisal-of-standardization-aetiopathogenesis-and-management-A-critical-review.pdf
- Siddiqi, A., Morkel, J. A., & Zafar, S. (2010). Antibiotic prophylaxis in third molar surgery: A randomized double-blind placebo-controlled clinical trial using a split-mouth technique. International Journal of oral and maxillofacial surgery, 39(2), 107-114. Abstract: https://pubmed.ncbi.nlm.nih.gov/20117915/
- Mamoun, J. (2017). Use of elevator instruments when luxating and extracting teeth in dentistry: clinical techniques. Journal of the Korean Association of Oral and Maxillofacial Surgeons, 43(3), 204-211. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5529197/
- Chiapasco, M., De Cicco, L., & Marrone, G. (1993). Side effects and complications associated with third molar surgery. Oral surgery, oral medicine, oral pathology, 76(4), 412-420. Abstract https://pubmed.ncbi.nlm.nih.gov/8233418/
- Valmaseda-Castellón, E., Berini-Aytés, L., & Gay-Escoda, C. (2001). Inferior alveolar nerve damage after lower third molar surgical extraction: a prospective study of 1117 surgical extractions. Oral Surgery, Oral Medicine, Oral Pathology, Oral Radiology, and Endodontology, 92(4), 377-383. Abstract: https://pubmed.ncbi.nlm.nih.gov/11598570/
- Bui, C. H., Seldin, E. B., & Dodson, T. B. (2003). Types, frequencies, and risk factors for complications after third molar extraction. Journal of Oral and Maxillofacial Surgery, 61(12), 1379-1389. Abstract: https://www.sciencedirect.com/science/article/abs/pii/S027823910300836X
- Blakey, G. H., Marciani, R. D., Haug, R. H., Phillips, C., Offenbacher, S., Pabla, T., & White Jr, R. P. (2002). Periodontal pathology associated with asymptomatic third molars. Journal of oral and maxillofacial surgery, 60(11), 1227-1233. Abstract: https://pubmed.ncbi.nlm.nih.gov/12420253/
- Normando, D. (2015). Third molars: To extract or not to extract?. Dental press journal of orthodontics, 20(4), 17-18. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4593524/
- Falci, S. G. M., De Castro, C. R., Santos, R. C., de Souza Lima, L. D., Ramos-Jorge, M. L., Botelho, A. M., & Dos Santos, C. R. R. (2012). Association between the presence of a partially erupted mandibular third molar and the existence of caries in the distal of the second molars. International Journal of oral and maxillofacial surgery, 41(10), 1270-1274. Abstract: https://pubmed.ncbi.nlm.nih.gov/22464852/
- Morant, H. (2000). NICE issues guidelines on wisdom teeth. BMJ: British Medical Journal, 320(7239), 890. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1117824/
- Faculty of Dental Surgery of the Royal College of Surgeons of England. Current clinical practice and parameters of care: the management of patients with third molar teeth. London: Faculty of Dental Surgery RCS (Eng), 1997.
- Friedman, J. W. (2007). The prophylactic extraction of third molars: a public health hazard. American journal of public health, 97(9), 1554-1559. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1963310/
- Stathopoulos, P., Mezitis, M., Kappatos, C., Titsinides, S., & Stylogianni, E. (2011). Cysts and tumors associated with impacted third molars: is prophylactic removal justified?. Journal of oral and maxillofacial surgery, 69(2), 405-408. Abstract: https://pubmed.ncbi.nlm.nih.gov/21050646/
- American Public Health Association. (2008). Opposition to prophylactic removal of third molars (wisdom teeth). Policy Statement Database. Policy, (2008). Full text: https://www.apha.org/policies-and-advocacy/public-health-policy-statements/policy-database/2014/07/24/14/29/opposition-to-prophylactic-removal-of-third-molars-wisdom-teeth
- American Association of Oral and Maxillofacial Surgeons. (2016). Management of Third Molar Teeth. Full text: https://www.aaoms.org/docs/govt_affairs/advocacy_white_papers/management_third_molar_white_paper.pdf
- Bouloux, G. F., Busaidy, K. F., Beirne, O. R., Chuang, S. K., & Dodson, T. B. (2015). What is the risk of future extraction of asymptomatic third molars? A systematic review. Journal of Oral and Maxillofacial Surgery, 73(5), 806-811. Abstract: https://www.joms.org/article/S0278-2391(14)01628-0/abstract
- McArdle, L. W. (2019). The prevention and management of distal cervical caries of the mandibular second molar. Dental Update, 46(5), 406-410. Full text: https://www.researchgate.net/profile/Louis_McArdle/publication/333226380_The_prevention_and_management_of_distal_cervical_caries_of_the_mandibular_second_molar/links/5ebe8b0b92851c11a867f606/The-prevention-and-management-of-distal-cervical-caries-of-the-mandibular-second-molar.pdf

 Dentures: Costs, Concerns and Care
Dentures: Costs, Concerns and Care