Table of Contents[Hide][Show]
Is something strange happening with your taste buds? Got a problem that’s on the tip of your tongue, prompting strange white spots, bizarre tastes, and cracked lips? The culprit might be oral thrush.
Don’t panic — managing oral thrush is easy with the right combination of medical intervention and natural remedies.
Here, you’ll find out how to recognize the signs of oral thrush and the risk factors that make you more susceptible to it. What’s more, we’ll give you a range of natural solutions for getting rid of discomfort quickly.
If you’re looking for a quick and easy solution to oral candida, you’ve come to the right place.
What is oral thrush?
Thrush is a byproduct of an infection caused by a yeast germ called Candida. The most common strain of this fungus is Candida albicans, also known as Candida or C. albicans.
This type of yeast infection is called oral candidiasis, oropharyngeal candidiasis, or just thrush. The Candida fungus is also the most frequent cause of penile and vaginal yeast infection.
The mouth is one of the most common sites of Candida infections, which leads to oral thrush. This fungus is also found within the digestive tract and vagina.
Small amounts of Candida are almost always present in the mouth, but oral thrush infections happen when an overgrowth of Candida occurs.
This overgrowth is what leads to the symptoms of oral thrush.
Chemical changes that lead to thrush can occur as a side effect of exposure to certain drug treatments, antibiotics, or specific medical conditions (like diabetes, for example).
Get Dr. B’s Dental Health Tips
You can’t be healthy without a healthy mouth. Sign up for my free newsletter and you’ll get my unconventional tips, starting with: If I had a cavity, here’s exactly what I’d do to reverse it.

14 Risk Factors & Causes of Oral Thrush
- Poor oral hygiene: Failing to brush your teeth, floss, and otherwise manage the balance of your oral microbiome can allow to fungal overgrowth.
- Being a baby: A baby’s mouth is more susceptible to oral thrush than older children, particularly if they use unsterilized pacifiers.
- Wearing dentures: Dentures require constant care. If you wear dentures that don’t fit properly, aren’t removed at night, and aren’t kept clean, this could cause Candida overgrowth.
- Excessive use of antibiotics: Antibiotics can kill harmless germs in the mouth, but they don’t kill Candida. This yeast can multiply faster when there are fewer commensal bacteria to fight against illness, which is why they’re linked with more frequent oral thrush. The same problem applies to excessively using an antibacterial mouthwash.
- Poor nutrition and a high sugar diet: Sugar is an easy source of food for Candida. Frequently eating high-carbohydrate and high-sugar foods can feed Candida and cause it to get out of control.
- Limited intake of vitamin B12, vitamin C, folate, or iron: All of these nutrients are effective for promoting a healthy digestive system. Without them, your internal balance can begin to falter, encouraging Candida’s development. Deficiencies are associated with higher rates of Candida infection, particularly in older adults.
- Exposure to steroid inhalers or tablets: Inhaled steroids, such as asthma inhalers, can promote growth of Candida yeast, making the problem worse over time.
- Dry mouth: Dry mouth can happen for many reasons, from mouth breathing to taking antidepressant medications, to having Sjogren’s syndrome or another medical condition that causes salivary deficiencies. Either way, a dry mouth makes you more predisposed to Candida overgrowth (and other bacterial overgrowth).
- Diabetes: Uncontrolled diabetes greatly increases your risk of oral candidiasis.
- Cushing’s syndrome
- Cancer: Not only does cancer weaken your body’s ability to fight infection, but cancer treatments like radiation and chemotherapy increase your risk of oral thrush.
- Immune System Conditions (HIV/AIDS and leukemia)
- Poor health or a weak immune system: Just like those with chronic illnesses, people with weak immune systems are far more likely to suffer from yeast, fungi, and parasitic infections.
- Smoking: Smoking creates an environment in the mouth that kills good bacteria but allows bad bacteria to thrive. This damages the natural balance needed to prevent Candida overgrowth.
Symptoms of Oral Thrush
Candida albicans is a form of opportunistic pathogenic yeast (yeast that causes disease in humans) that leads to plenty of problems.
It is usually divided into three types, depending on the appearance of the infection:
- Pseudomembranous: This is considered “classic” oral thrush and presents with typical “cottage cheese” lesions.
- Erythematous (atrophic): Instead of white patches, the overgrowth causes raw, red patches within the mouth.
- Hyperplastic: Sometimes called “plaque-like candidiasis” or “nodular candidiasis”, this is most common in patients with HIV infection. A hard-to-remove plaque exists with this variation and is rare and much harder to get rid of.
Common symptoms of oral thrush might include:
- A collection of red or white lesions in the mucous membranes (wet tissue) of your mouth that may join together to form larger white patches. Sometimes they change color to gray or yellow, and if you wipe away a spot the underlying skin may be red. These lesions are generally raised and are often described to look like cottage cheese. They usually show up on the tongue and inner cheeks, and may spread out to the roof of your mouth, gums, tonsils, or even the back of your throat.
- Areas in your mouth might be uncomfortable, sore, or have a burning sensation without the presence of white spots. This happens frequently when you develop oral thrush after taking steroids or antibiotics.
- You might notice soreness or cracked skin around the outside of your mouth — mainly at the corners where the upper and lower lips meet.
- Denture-wearers may notice persistent redness or soreness under a denture.
- Many cases of oral thrush are painless. However, the condition can cause soreness that makes eating and drinking uncomfortable. Babies often drool and struggle to feed properly because of the discomfort.
- Some people notice that their taste is affected.
- You may notice a dry, cotton-mouth sensation.
In severe cases, oral thrush spots can spread into the esophagus (called esophageal candidiasis), causing:
- Pain when swallowing or talking
- Difficulty swallowing, and/or the sensation of something being stuck in the throat
- Fever
- Babies with oral thrush can pass the infection to their mothers during breastfeeding, causing intense itching and pain in the nipples.
Nursing mothers may experience the following symptoms:
- Shiny or flaking skin around the nipple
- Severe pain during breastfeeding
- Piercing pain throughout the breast
If you experience an infection that occurs after breastfeeding, the best way to clear it up fast is an antifungal cream like clotrimazole (Lotrimin) or terbinafine (Lamisil).
In an ideal world, we’d all keep Candida in check with our natural balance of good and bad bacteria. Unfortunately, we’re often exposing the bacteria in our mouths to factors that upset the balance. For some people, thrush can make the mouth too sensitive for regular oral hygiene, which only upsets the balance further.
Whether your symptoms are minimal or severe, it’s important to seek help, as when left untreated, some studies show that oral thrush weakens the immune system.
What’s more, in people with weakened immune systems, Candida can enter the bloodstream and spread. This process can cause problems in various parts of the body, including the liver, heart, and brain.
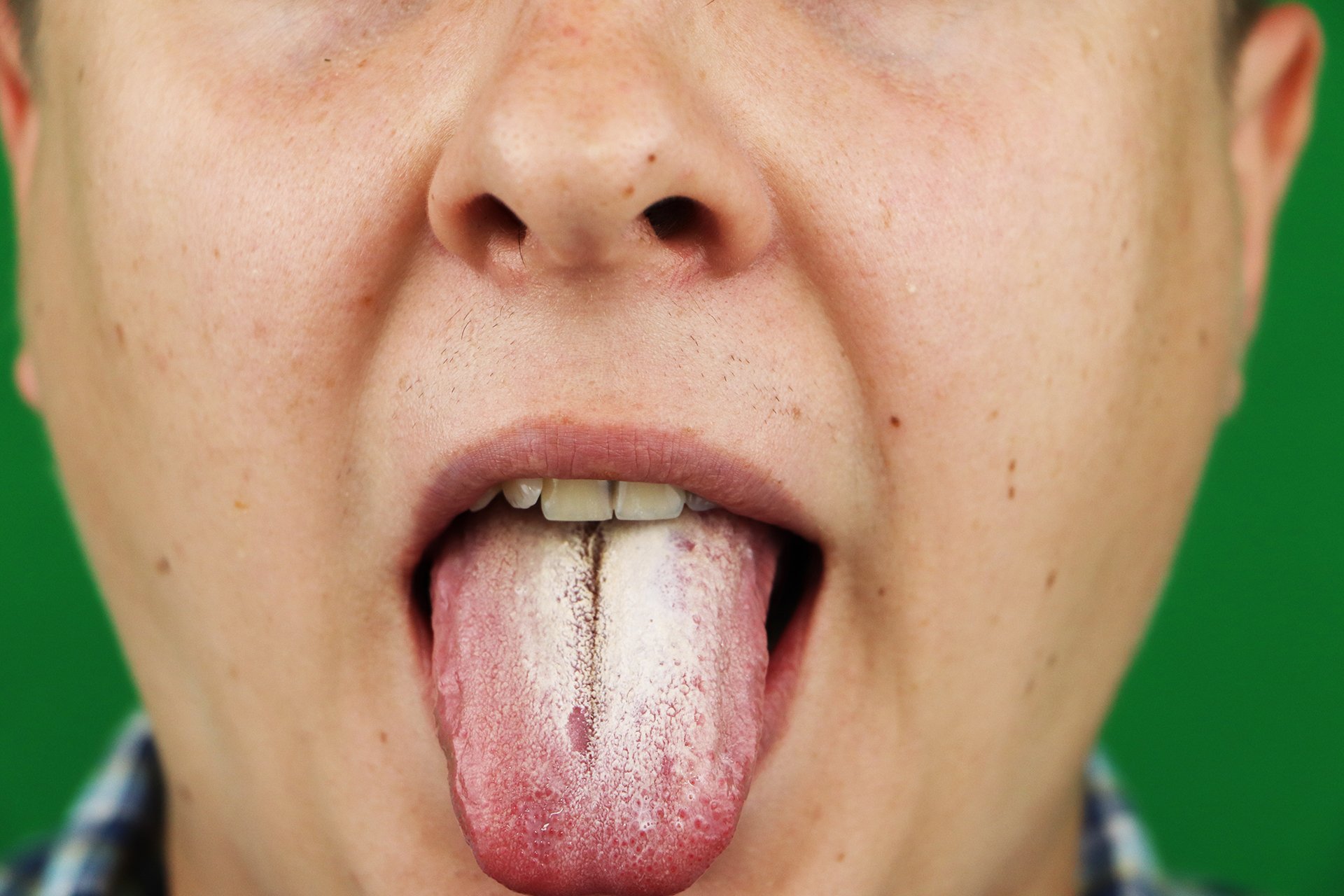
What does oral thrush look like?
Below are images of some examples of oral thrush. Just click the plus sign (+) to view the image.
References
References
How Your Doctor or Dentist Diagnoses Candida
You might think that diagnosing oral thrush symptoms would be easy — particularly in mouths covered with white spots. But remember, that’s not always the case.
In babies, doctors scrape the baby’s tongue to detect Candida. For adults, the same tests can apply, but oral thrush can mimic the symptoms of various illnesses and diseases. Some Candida symptoms appear similarly to the earlier stages of cancer, making it difficult to pinpoint a cause.
Conditions that may need be ruled out in order to diagnose thrush include:
- Angular cheilitis: An inflammatory condition, usually in the corners of the mouth
- Median rhomboid glossitis (MRG): Sometimes known as atrophic tongue, it’s related to Candida and causes a red, flat, raised lesion on the middle and/or back section of the tongue and is not associated with the same risk factors as thrush
- Linear gingival erythema: Commonly associated with HIV infection, this condition is an inflammatory condition of the gums. Candida in patients with HIV/AIDS can eventually lead to linear gingival erythema, although they are separate conditions.
Some doctors will suggest blood tests to examine conditions that make you more susceptible to oral thrush. For instance, they might use a blood test to check for levels of folate, vitamin B12, vitamin C, and iron.
Occasionally, doctors will need a biopsy to confirm an oral thrush diagnosis. Suspicion of esophageal candidiasis may necessitate a throat swab culture or an endoscopy.
Treatments for Oral Thrush
Fortunately, treatment for oral thrush is usually quite straightforward.
For babies, the matter can clear up spontaneously. Mothers can prevent further infection by sterilizing mouth toys and feeding equipment.
For adults, it’s crucial to find the condition that causes the thrush. That might mean adjusting diabetes treatments or investing in better-fitting dentures.
For mild cases of oral thrush, the usual treatment is nystatin (Nyamyc), which is a topical application that is in liquid drop form. Miconazole mouth gel or lozenges are also fairly effective but may lead to vomiting or diarrhea.
Tablets containing the common antifungal medications fluconazole (Diflucan) or itraconazole (Sporanox) can also clear fungal infections from the body. Tablets are often prescribed for more severe cases.
In complex cases, systemic treatments are offered through antifungal tablets and injections.
If you don’t respond to the typical treatments, you may need to alter your medications and your health care provider may refer you to a specialist.
Remember: The best way to avoid getting re-infected is to change the conditions that caused the overgrowth of Candida in the first place.
Ways to Prevent Oral Thrush
Most of the time, overcoming oral problems is about maintaining good hygiene. Learning proper brushing and flossing techniques while maintaining a healthy diet can limit your risk of Candida overgrowth.
To limit your risk of oral thrush:
- Practice good oral hygiene by brushing twice a day, flossing at least once a day, and scraping your tongue.
- Get regular checkups with your dentist. This is particularly important if you have dentures or have diabetes.
- Treat chronic health issues. Conditions like diabetes and HIV can easily disturb the bacterial balance in your body, leading to oral thrush. Make sure you take your medications exactly as directed.
- Don’t overuse antibiotics.
- Avoid conventional mouthwash, which not only disrupts your oral microbiome’s balance but also dries out your mouth and leaves you at an even greater risk of thrush. Ask your dentist if you’re concerned about the natural bacteria balance in your mouth.
- Clean inhalers after you use them.
- Limit foods rich in yeast and sugar. These will lead to extra Candida growth.
- If you are a smoker, ask for help with quitting.
4 Home Remedies for Oral Thrush
If you can’t handle the soreness or other symptoms of oral thrush for another second, natural solutions might offer a reprieve. These solutions are effective at minimizing some of the most uncomfortable symptoms of Candida:
1. Essential Oils
Various essential oils are as effective as antifungals. When mixed with water, they’re ideal for swishing around your mouth to reduce symptoms.
Keep in mind that essential oils should only be used in the mouth for a short period of time, as they may kill good bacteria along with the bad. Once your thrush is resolved, avoid strong bactericidal/antifungal compounds like these.
For instance, clove oil is just as effective as nystatin — a drug frequently prescribed to manage oral thrush.
Oregano oil can also kill bacteria quickly, and it’s got quite a nice taste, too — just make sure to dilute it a lot, as undiluted oregano oil will burn soft tissue. A study published in 2010 found that oregano oil was a powerful alternative oral thrush treatment.
Myrrh oil can kill a variety of different fungi and parasites, including Candida. Studies have found that when mixed with toothpaste, myrrh controls Candida overgrowth.
2. Apple Cider Vinegar Oral Rinses
Apple cider vinegar (ACV) may help to regulate the presence of Candida while restoring the natural pH level in the mouth. Since apple cider vinegar has a pretty strong taste, you might need to dilute it with water to sip throughout the day. It’s best to avoid trying to gulp it all down at once.
If you wear dentures, soaking them in ACV overnight may help to kill Candida that would otherwise stick around on your dental appliance.
Try this recipe for banishing bad breath with apple cider vinegar. Since a poor pH balance can often lead to halitosis (bad breath), an apple cider rinse may solve two problems at once.
3. Probiotics
Adding probiotic foods, cultured dairy, and/or oral probiotics into your routine can help to kill the Candida overgrowth in your body. This substance promotes the natural restoration of good bacteria in your system and can keep Candida in check. In other words, it returns balance to your mouth.
4. Coconut Oil
Coconut oil possesses several great antimicrobial properties. The combination of caprylic and lauric acid found in coconut oil helps to kill off excess Candida. You can use it topically or mix it with food.
Studies have found that coconut oil is just as effective as fluconazole (a common Candida medication) against thrush symptoms.
Caprylic acid, one of the major components of coconut oil, may be powerful against Candida infection on its own.
For another perspective on curing candida in the mouth, read this guest post by Amie Valpone, who shares her advice and experience with candida.
Is thrush contagious?
While yeast/candidal infections are not always contracted through direct contact, it is possible to pass that Candida overgrowth.
If you have oral thrush, you can pass it to someone else via kissing or oral sex. A vaginal or penile yeast infection may be contagious during anal, oral, or vaginal sex and can present as oral thrush, even if it started elsewhere.
Mothers may pass vaginal yeast infections to babies as oral thrush during delivery or breastfeeding.
Although Candida infections can be contagious, having any sort of yeast infection does not necessarily mean you contracted it from another person.
Key Takeaways: Oral Thrush
Candida overgrowth is a common problem for many people. The important thing to remember is that you can fight back and regain good oral health! The information outlined above will help you to get back on your feet and overcome discomfort fast!
4 Steps to Cure Candida in the MouthReferences
- Patil, S., Rao, R. S., Majumdar, B., & Anil, S. (2015). Clinical appearance of oral Candida infection and therapeutic strategies. Frontiers in microbiology, 6, 1391. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4681845/
- Akpan, A., & Morgan, R. (2002). Oral candidiasis. Postgraduate medical journal, 78(922), 455-459. Full text: https://www.researchgate.net/profile/Asangaedem_Akpan/publication/11202693_Oral_Candidiasis/links/02e7e52135e018185f000000/Oral-Candidiasis.pdf
- Paillaud, E., Merlier, I., Dupeyron, C., Scherman, E., Poupon, J., & Bories, P. N. (2004). Oral candidiasis and nutritional deficiencies in elderly hospitalised patients. British Journal of Nutrition, 92(5), 861-867. Abstract: https://www.ncbi.nlm.nih.gov/pubmed/15533276
- Challacombe, S. J. (1986). Haematological abnormalities in oral lichen planus, candidiasis, leukoplakia and nonspecific stomatitis. International journal of oral and maxillofacial surgery, 15(1), 72-80. Abstract: https://www.ncbi.nlm.nih.gov/pubmed/3083007
- Lamster, I. B., Lalla, E., Borgnakke, W. S., & Taylor, G. W. (2008). The relationship between oral health and diabetes mellitus. The Journal of the American Dental Association, 139, 19S-24S. Abstract: https://www.ncbi.nlm.nih.gov/pubmed/18809650
- Peterson, D. E. (1992). Oral candidiasis. Clinics in geriatric medicine, 8(3), 513-528. Abstract: https://www.ncbi.nlm.nih.gov/pubmed/1504942
- Goregen, M., Miloglu, O., Buyukkurt, M. C., Caglayan, F., & Aktas, A. E. (2011). Median rhomboid glossitis: a clinical and microbiological study. European Journal of dentistry, 5(4), 367. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3170022/
- Seneviratne, C. J., & Jayasinghe, R. D. (2015). Association of Candida with Linear Gingival Erythema in HIV-Infected Subjects. In Oral Candidosis (pp. 83-94). Springer, Berlin, Heidelberg. Abstract: https://link.springer.com/chapter/10.1007/978-3-662-47194-4_12
- Chee, H. Y., & Lee, M. H. (2007). Antifungal activity of clove essential oil and its volatile vapour against dermatophytic fungi. Mycobiology, 35(4), 241-243. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3763181/
- Cleff, M. B., Meinerz, A. R., Xavier, M., Schuch, L. F., Meireles, M. C. A., Rodrigues, M. R. A., & Mello, J. R. B. D. (2010). In vitro activity of Origanum vulgare essential oil against Candida species. Brazilian Journal of Microbiology, 41(1), 116-123. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3768597/
- Adwan, G., Salameh, Y., Adwan, K., & Barakat, A. (2012). Assessment of antifungal activity of herbal and conventional toothpastes against clinical isolates of Candida albicans. Asian Pacific journal of tropical biomedicine, 2(5), 375-379. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3609312/
- Pinto, T. M. S., Neves, A. C. C., Leão, M. V. P., & Jorge, A. O. C. (2008). Vinegar as an antimicrobial agent for control of Candida spp. in complete denture wearers. Journal of Applied Oral Science, 16(6), 385-390. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4327708/
- Hasslöf, P., Hedberg, M., Twetman, S., & Stecksén-Blicks, C. (2010). Growth inhibition of oral mutans streptococci and candida by commercial probiotic lactobacilli-an in vitro study. BMC oral health, 10(1), 18. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2908555/
- Ogbolu, D. O., Oni, A. A., Daini, O. A., & Oloko, A. P. (2007). In vitro antimicrobial properties of coconut oil on Candida species in Ibadan, Nigeria. Journal of medicinal food, 10(2), 384-387. Abstract: https://www.ncbi.nlm.nih.gov/pubmed/17651080
- Omura, Y., O’Young, B., Jones, M., Pallos, A., Duvvi, H., & Shimotsuura, Y. (2011). Caprylic acid in the effective treatment of intractable medical problems of frequent urination, incontinence, chronic upper respiratory infection, root canalled tooth infection, ALS, etc., caused by asbestos & mixed infections of Candida albicans, Helicobacter pylori & cytomegalovirus with or without other microorganisms & mercury. Acupuncture & electro-therapeutics research, 36(1-2), 19-64. Abstract: https://www.ncbi.nlm.nih.gov/pubmed/21830350


 Wisdom Teeth: Pictures, Symptoms, Surgery, & Pain Relief
Wisdom Teeth: Pictures, Symptoms, Surgery, & Pain Relief