Table of Contents[Hide][Show]
Is a tongue tie, an issue with the frenulum of the tongue, the source of your child’s breastfeeding or speech issues?
For a long time, people just didn’t seem to know much about tongue ties. In the early years of my practice, few of my patients had ever heard of it! When I pointed out that they or their children might be tongue tied, I was often the very first practitioner who’d mentioned it to them.
When I told them that a tongue tie might actually be the root cause of their oral myofunctional issues, or even their sleep apnea, I’m sure that some of them thought I was crazy.
But in the last few years, tongue ties have gained center stage as more families put an emphasis on the importance of breastfeeding.
Diagnoses have been skyrocketing. Dentists and orthodontists also began reaching out more frequently to discuss the application of myofunctional therapy exercises to tongue tie treatment. Today, that little bit of interest has become a surge of awareness.
Tongue ties and their impact on health and craniofacial development are finally becoming mainstream. This is great news, because it means that fewer people will suffer from undiagnosed and untreated symptoms of a tongue tie.
Catching and treating a tongue tie early is vitally important, so in this article, I’ll cover everything parents need to know about tongue ties.
What is a tongue tie?
Tongue tie is the improper development of the anchoring of the tongue to the mouth, which results in limited tongue movement. The frenulum, which is what attaches the tongue to the floor of the mouth, is too short, too thin, or too tight to allow for proper tongue use.
Being tongue tied isn’t just a figure of speech—it’s a very real medical condition. Tongue tie affects oral and facial development and has a range of other serious health consequences that may not appear for decades.
We all have a lingual frenulum (or frenum) under our tongue. If you lift your tongue and look in the mirror, you’ll see it. The frenum is the tissue that connects the tongue to the floor of the mouth.
Normal lingual frenulum function means that the tongue, with the mouth closed, rests on the top of the mouth and touches the back of the front teeth.
In some people, the frenum is tighter or thicker than it should be, which can physically restrict the movement of the tongue.
A tongue tie can also be referred to as ankyloglossia, short frenum, anchored tongue, or tethered oral tissue (TOT).
Get Dr. B’s Dental Health Tips
You can’t be healthy without a healthy mouth. Sign up for my free newsletter and you’ll get my unconventional tips, starting with: If I had a cavity, here’s exactly what I’d do to reverse it.

How to Diagnose a Tongue Tie in Babies, Children, or Adults (with Pictures)
There are a few ways to classify or identify tongue ties, but it’s an art, not a science—and experts don’t agree on diagnostic criteria. Not all tongue ties can be seen with the naked eye, and some “normal” looking tongues suffer from limited range of motion and must be treated.
That’s why it’s important, ultimately, to have a tongue tie diagnosed by a pediatrician, ENT physician, dentist, myofunctional therapist, or board-certified lactation consultant.
The assessment tool developed by Kotlow can be useful in classifying severity of a tongue tie, although this isn’t the only diagnostic tool available. It defines the distance of the tie to the tip of the tongue:
- Class 1: Mild, 12-16 millimeters
- Class 2: Moderate, 8-11 millimeters
- Class 3: Severe, 3-7 millimeters
- Class 4: Complete, less than 3 millimeters
Another way to classify tongue ties include looking for anterior or posterior ties. Anterior ties would be all four classes named above, which are visible and measurable, while a posterior tie lies beneath the mucous membranes in the bottom of the mouth. You can only diagnose a posterior tongue tie by touch.
The system developed by Hazelbaker in the 1990s uses slightly different measurements and includes additional information to identify ties:
- Type 1, 100% Tongue-Tie: Anterior tongue tie less than 2 millimeters from the tip, attached to the alveolar ridge, frenulum can be thin, thick, restricted, or elastic
- Type 2, 75% Tongue-Tie: Anterior tongue tie, 2-5 millimeters from tip, attached to the alveolar ridge, or base of ridge/mouth floor, frenulum may be tin, thick, restricted, or elastic
- Type 3, 50% Tongue-Tie: Mid tongue tie, 6-10 millimeters from tip, attached to alveolar ridge/mouth floor, frenulum may be thin or thick but is more restricted, as more of the tongue is “free”
- Type 4, 25% Tongue-Tie: Posterior tongue tie, 11-15 millimeters from tip, attached to mouth floor/base of alveolar ridge or on the alveolar ridge, frenulum may be thin or thick but is less restricted
- Type 5, Submucosal Tongue-Tie: Posterior tongue tie, more than 15 millimeters from tip, attached to mouth floor or base of alveolar ridge, frenulum is typically thin and shiny when tongue is lifted
The method developed in the UK by Griffiths et al used classification by three visual appearances of the frenulum:
- Diaphanous (transparent)
- Medium (not transparent)
- Thick (chunky)
Other identifiers used to check for tongue ties in newborn babies include:
- Heart-shaped tongue
- “Eiffel tower” frenum
- Lip ties (scroll down for more on this)
- Unusually thick frenum
- Nipple pain or other breastfeeding difficulties, especially when accompanied by a “clicking” as baby attempts to latch
- Prolonged drooling
- Difficulty raising the tongue, moving it sideways, or sticking out the tongue
In older children or adults, tongue tie can cause symptoms like:
- Speech difficulties
- Problems with eating, such as issues licking an ice cream cone
- Inability to stick out the tongue beyond the upper lip
- Issues kissing with tongue
Here are three examples of tongue ties to help you identify them:
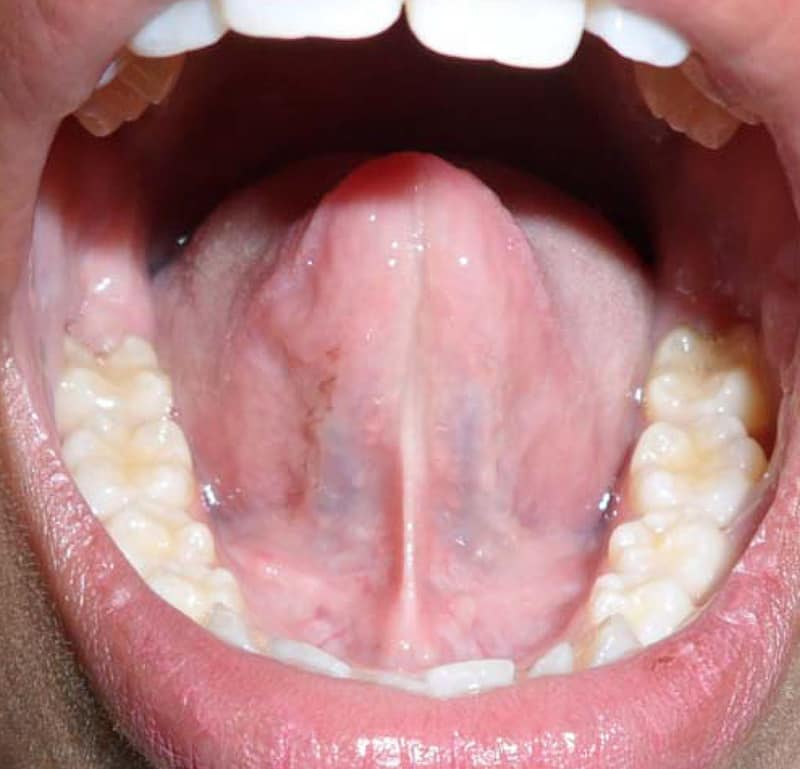


8 Symptoms of Tongue Tie
As a myofunctional therapist, the position of the tongue is my key focus. Symptoms that arise from tongue tie are far-reaching and can affect not only breastfeeding but the rest of a person’s life.
The tongue should rest in the top of the mouth, filling up the entire palate from front to back. When the tongue is resting in the correct position, it shapes the maxilla (upper jaw) and guides the growth of the face. The tongue also provides an internal support system for the upper jaw.
But if a person is tongue tied, their tongue may not be able to reach the top of the mouth because it’s physically restricted. This causes the palate to develop smaller and narrower, and the teeth to grow in crooked. Also, the mandible (lower jaw) is often smaller and set back, and the airway is restricted.
Because of this, children who grow into adults without having their tongue tie treated often experience a range of oral myofunctional symptoms, including:
- Speech issues
- Mouth breathing
- Jaw pain, clenching, and grinding
- Headaches
- Head, neck, and shoulder tension
- Forward head posture
- Snoring, sleep disordered breathing, Upper Airway Resistance Syndrome (UARS), and sleep apnea
- Increased risk of cavities and gum disease
- Slower orthodontic treatment
- Orthodontic relapse
Let’s take a look at the eight most significant issues that arise from a tongue tie.
1. Breastfeeding Problems
Breastfeeding is one of the first ways a tongue tie can be noticed.
When mothers have trouble breastfeeding, a tongue tie can often be to blame. The baby’s tongue is unable to make a “vacuum” on the breast because it can’t reach the lower gum, resulting in issues with latching.
This leads many parents to resort to bottle feeding or to deal with several days or weeks of painful, frustrating breastfeeding. In extreme cases, a baby can have failure to thrive after mom’s milk supply has dropped or baby has been unable to latch.
However, if babies are bottle fed from the beginning, or meet weight-gain and growth markers, the tongue tie can be missed or overlooked.
Just because a mother managed to breastfeed her baby doesn’t mean that tongue tie isn’t an issue.
Many times, a nurse or lactation consultant will notice a tongue tie but not recommend a release because the breastfed baby is able to gain weight. Unfortunately, issues like mastitis or low milk supply can still occur.
A 2017 Cochrane review found that the release of a tongue tie via frenectomy improved the mother’s pain, but didn’t have a significant effect on breastfeeding success overall. However, a clinical trial published later the same year found that clipping a tongue tie does improve breastfeeding outcomes over the first month after the procedure.
Why does this matter? For one, breastfeeding is important for the development of the mouth, jaw, and entire oral structure. It’s also helpful in bonding between mom and baby.
Not every woman is able to breastfeed, and that’s okay. However, if you can and choose to do so, it will generally help in many ways including the development of your baby’s mouth.
Ideally, correcting a tongue tie before the 72-hour mark seems to have the most positive impact on breastfeeding.
From a myofunctional perspective, the tongue tie still needs to be released so that proper oral development can take place.
2. Speech Difficulties
A tongue tie can certainly affect a child’s speech, but this may not always happen.
Sometimes, doctors and dentists are reluctant to release a tongue tie if it hasn’t been pointed out as problematic by a speech-language pathologist. However, as I explained above, it comes down to much more than speech—growth and development of the jaws and teeth will be impacted by a tongue tie.
The most common sounds that kids struggle with if they are tongue tied are “r” and “l”. If your child has these specific speech issues, the first thing I’d recommend would be to screen for a tongue tie.
Even after an older child has undergone frenectomy, s/he will likely require speech therapy to correct any habitual speech difficulties.
3. Improper Jaw/Facial Growth
Like Dr. Burhenne, I encourage parents to do what they can to support the best possible growth of the face, jaw, and mouth. This can be done by introducing vitamin K2 in the diet as early as preconception, as well as breastfeeding and minimizing the use of pacifiers and sippy cups.
Why? Because the more you can support your child’s orofacial growth, the lower their chances will be for orthodontic treatment later in life.
Before the year 1940 or so, it wasn’t unusual to see midwives snip a tongue tie immediately upon noticing it. This was generally to support the baby’s ability to breastfeed.
Interestingly, it was during the following decades that the need for orthodontic treatment skyrocketed. This can be attributed to a number of factors, not least of which is the lack of nutrients in the standard American diet. However, it’s possible that tongue tie is partly to blame.
Untreated tongue tie leads to issues with orofacial growth, according to multiple studies. To help your child avoid the need for costly treatment such as braces, it’s a good idea to get rid of tongue ties early.
4. Sleep Disorders
While it might sound unrelated, tongue tie can lead, sometimes decades into life, to issues with sleep.
When children have an abnormally short frenulum, they are much more likely to mouth breathe during sleep. During the first two years of life, the poor tongue position may lead to development of an abnormally small palate and/or airway. These developmental problems very frequently cause disordered sleep breathing, like sleep apnea.
Because sleep apnea in children often presents like ADHD, I suggest you do the following if you know your child has symptoms of ADHD and/or sleep issues:
- Talk to your healthcare professional about having a sleep study conducted to look for sleep apnea or other sleep-disordered breathing and determine a treatment plan if necessary
- Have your pediatrician or dentist examine for tongue tie and snip it if present
- Schedule an appointment with a myofunctional therapist to recover full range of motion after frenectomy (otherwise, your child may still mouth breathe during sleep from muscle memory)
Sleep apnea in adulthood is associated with a large number of related chronic health conditions, so it shouldn’t be left untreated.
5. TMJ Pain
Since individuals with tongue tie don’t have optimal mouth position, more pressure may be constantly applied to the TMJ muscle. This could lead to a TMJ disorder, which can be quite painful.
Cases of TMJ can also manifest as migraines in addition to jaw pain.
When clipping the frenulum, myofunctional therapy is important to stretching and developing better motion for the TMJ and attached muscles.
6. Slowed Orthodontic Treatment and Orthodontic Relapse
Since the position of the teeth are so impacted by the existence of a tongue tie, many sufferers need orthodontic treatment. But since the tongue can’t move properly, orthodontic treatment may take a longer time.
In addition, tongue tie makes orthodontic relapse, or the movement of teeth away from their reset position after braces/orthodontics, more likely.
7. Problems with Oral Hygiene
Ever tried brushing your teeth without being able to move your tongue? Try it—you’ll discover it’s far from easy.
When the tongue’s motion is limited, it creates difficulty in brushing food debris away from teeth and disorganizing the biofilm. Bacteria may also be caught in the space created by the anchored tongue.
All of these conditions can lead to inflammation and tooth decay. Not only can this translate to painful cavities or gum disease, but a tongue tie that has not been released makes for more uncomfortable dental appointments.
8. Suboptimal Digestion
The mouth is the gateway to the rest of the body and serves as the first step in the digestive process. When you’re unable to properly chew food, digestion is limited.
Over time, this can lead to poor digestion and related issues, like nutrient deficiencies, food sensitivities, and leaky gut.
Tongue Tie Causes and Risk Factors
What causes a tongue tie? The answer is still unclear.
Recent research is showing that tongue ties are linked to a mutation in the MTHFR gene. The science behind this is quite complicated but basically, what’s happening is that a specific gene isn’t quite working as it should.
In this case, the mutation involves a process known as “methylation”, which affects the body’s ability to deal with folate—an important element in prenatal nutrition. Tongue ties are just one of many conditions linked to this mutation. (Click here to get tested for an MTHFR gene mutation.)
Because tongue tie is linked to a genetic cause, it was once thought to be hereditary. I see this a lot in my practice; parents will reach out to me for help with a tongue tied child, only to find out that they’re tongue tied as well.
Interestingly, though, heritability of tongue tie hasn’t been well-established. In fact, some sources find no statistically significant family heritability for it at all.
Boys are more likely than girls to be born with tongue ties.
Treatment for Tongue Tie: Surgery & Myofunctional Therapy
Surgical Procedures for Tongue Tie
In most cases, tongue ties are treated with a minor surgical procedure to release the tie. This procedure is called a frenectomy but is also known as a frenotomy or frenulectomy.
The frenectomy is a simple, very low-risk procedure that only takes a few minutes. It’s usually done in-office by a dentist or ENT using a laser, scalpel, or sterile scissors without general anesthesia.
I recommend finding a specialist who’s very experienced at performing the procedure. If it’s not done correctly, or released enough, there’s a high chance the frenectomy will need to be done again.
For severe cases in older children or adults, a frenuloplasty might be required. This is a more complex version of the tongue tie surgery that does require general anesthetic.
After the frenectomy, caring for the wound is also critical. The mouth and tongue are great at healing, so it’s possible that the tongue will reattach, meaning it will literally heal back down the way it was.
So, I meet with my patients immediately following the release to guide them through caring for the wound and to teach them new gentle exercises. This allows the tissues to heal without reattaching and affecting the end result.
It’s often covered by insurance, but the cost of a frenectomy (tongue tie surgery) is somewhere between $795-2729.
Myofunctional Therapy for Tongue Tie and Why It Matters
There’s more to treating a tongue tie than just releasing it, and this is where myofunctional therapy comes in.
It’s very important to do myofunctional therapy exercises for at least 4-6 weeks before the frenectomy. This helps prepare for the procedure by strengthening the muscles of the tongue.
Once the tongue tie has been released, it’s time to train the tongue to move properly. Just because the tongue is now capable of a normal range of motion doesn’t mean it will be able to move the way it should.
Think of it like this—if your arm had been in a sling for a year, and you removed the sling one morning, your arm muscles would be weak and uncoordinated. You’d need to do some rehabilitation using physical therapy to strengthen the muscles.
In this case, the tongue has literally been tied down. It’s never moved or rested the way it should, but with myofunctional therapy, we can train it to rest in the correct position, and to move correctly in the mouth.
Without these exercises, it’s entirely possible that the tongue will never regain its full range of motion.
Consequences of Untreated Tongue Ties
Given the list of possible symptoms connected to a tongue tie, and how easy the surgery is, if a tongue tie has been diagnosed in a child, in my opinion it’s always worth releasing it.
It’s difficult to predict exactly how a tongue tie could affect the growth of the face and jaw, or what the other potential health effects could be. However, a tongue tie always has some impact on craniofacial development and overall health.
It’s definitely possible that the negative effects of a tongue tie will only become obvious in adulthood. Basically, adults who are tongue tied have compromised orofacial development and airways. This puts them in high-risk categories for myofunctional problems.
Often, the adults I work with have jaw pain and headaches or sleep apnea that are linked to unreleased tongue ties. Most times, these patients have no idea they were tongue tied to begin with.
Lip Ties
A lip tie is similar to a tongue tie, and the two are often seen together.
With lip ties, the small seams that we all have on the midline between our lips and gums are too short or thick, causing restricted lip movement. This can have a major impact on breastfeeding and speech, as well as dental development.
Lip-ties are treated exactly the same way as a tongue tie; the tie is surgically released, and myofunctional therapy exercises are prescribed.
This condition is less common than tongue tie, but almost every time you see a lip tie, you will also see a tongue tie.
Tongue Tie in Adults: Should adults have theirs released?
As I mentioned above, if a tongue tie has been diagnosed, it’s definitely worth having it released.
Some tongue tied adults may have few or even no symptoms for most of their life. But then out of the blue, they start having problems. The thing is…their symptoms didn’t just appear. They accumulated over decades of living with a compromised orofacial structure.
The body is an amazing organism, and it will do its very best to maintain health, but after enough time passes, things can start to go wrong.
It’s never too late to have a tongue tie released and to benefit from myofunctional therapy.
Key Takeaways: Tongue Tie
I hope this article has helped clarify what a tongue tie is, and why it’s so important to take this condition seriously.
If I could sum up my experience with tongue ties, I’d say that the adults I meet who are tongue tied always wish they had known about it sooner. They also wish that their parents had known about tongue ties, and that they were able to get treatment earlier in life.
Are the parent of a child with a tongue tie? I urge you to find an experienced practitioner to perform the release, and a myofunctional therapist to work with before and after. Proper treatment really does make a huge difference!
Sarah Hornsby, RDH
Pacifier Pros and Cons: When and How to Use Baby Pacifiers
References
- Walsh, J., Links, A., Boss, E., & Tunkel, D. (2017). Ankyloglossia and lingual frenotomy: national trends in inpatient diagnosis and management in the United States, 1997-2012. Otolaryngology–Head and Neck Surgery, 156(4), 735-740. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6475619/
- Segal, L. M., Stephenson, R., Dawes, M., & Feldman, P. (2007). Prevalence, diagnosis, and treatment of ankyloglossia: methodologic review. Canadian Family Physician, 53(6), 1027-1033. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1949218/
- Crippa, R., Paglia, M., Ferrante, F., Ottonello, A., & Angiero, F. (2016). Tongue-tie assessment: clinical aspects and a new diode laser technique for its management. Eur J Paediatr Dent, 17(3), 220-222. Full text: https://pdfs.semanticscholar.org/f139/742a3859c5ed17f277bd74fa61d1b1dddda8.pdf
- Hong, P., Lago, D., Seargeant, J., Pellman, L., Magit, A. E., & Pransky, S. M. (2010). Defining ankyloglossia: a case series of anterior and posterior tongue ties. International journal of pediatric otorhinolaryngology, 74(9), 1003-1006. Abstract: https://www.ncbi.nlm.nih.gov/pubmed/20557951
- Todd, D. A., & Hogan, M. J. (2015). Tongue-tie in the newborn: Early diagnosis and division prevents poor breastfeeding outcomes. Breastfeeding Review, 23(1), 11. Full text: https://www.researchgate.net/profile/David_Todd/publication/275357598_Tongue-tie_in_the_newborn_Early_diagnosis_and_division_prevents_poor_breastfeeding_outcomes/links/5b6152f80f7e9bc79a72d204/Tongue-tie-in-the-newborn-Early-diagnosis-and-division-prevents-poor-breastfeeding-outcomes.pdf
- O’Shea, J. E., Foster, J. P., O’Donnell, C. P., Breathnach, D., Jacobs, S. E., Todd, D. A., & Davis, P. G. (2017). Frenotomy for tongue‐tie in newborn infants. Cochrane Database of Systematic Reviews, (3). Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6464654/
- Ghaheri, B. A., Cole, M., Fausel, S. C., Chuop, M., & Mace, J. C. (2017). Breastfeeding improvement following tongue‐tie and lip‐tie release: A prospective cohort study. The Laryngoscope, 127(5), 1217-1223. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5516187/
- Todd, D. A., & Hogan, M. J. (2015). Tongue-tie in the newborn: Early diagnosis and division prevents poor breastfeeding outcomes. Breastfeeding Review, 23(1), 11. Full text: https://www.researchgate.net/profile/David_Todd/publication/275357598_Tongue-tie_in_the_newborn_Early_diagnosis_and_division_prevents_poor_breastfeeding_outcomes/links/5b6152f80f7e9bc79a72d204/Tongue-tie-in-the-newborn-Early-diagnosis-and-division-prevents-poor-breastfeeding-outcomes.pdf
- Srinivasan, B., & Chitharanjan, A. B. (2013). Skeletal and dental characteristics in subjects with ankyloglossia. Progress in orthodontics, 14(1), 44. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4384905/
- Vaz, A. C., & Bai, P. M. (2015). Lingual frenulum and malocclusion: An overlooked tissue or a minor issue. Indian Journal of Dental Research, 26(5), 488. Full text: https://pdfs.semanticscholar.org/7dae/a10de8d5db9f49035e3a4e97974de0ee7ba0.pdf
- Huang, Y. S., Quo, S., Berkowski, J. A., & Guilleminault, C. (2015). Short lingual frenulum and obstructive sleep apnea in children. Int J Pediatr Res, 1(003). Full text: https://pdfs.semanticscholar.org/a135/63cf5f212e8676416c7d722e9dd89393fc37.pdf
- Halbower, A. C., Degaonkar, M., Barker, P. B., Earley, C. J., Marcus, C. L., Smith, P. L., … & Mahone, E. M. (2006). Childhood obstructive sleep apnea associates with neuropsychological deficits and neuronal brain injury. PLoS medicine, 3(8), e301. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1551912/
- Jang, S. J., Cha, B. K., Ngan, P., Choi, D. S., Lee, S. K., & Jangf, I. (2011). Relationship between the lingual frenulum and craniofacial morphology in adults. Full text: http://dentistry.wvu.edu/media/1173/relationship-between-the-lingual-frenulum-and-craniofacial-morphology-in-adults.pdf
- Sari, L. N. I., & Auerkari, E. I. (2018, May). Molecular Genetics and Epigenetics of Ankyloglossia. In 11th International Dentistry Scientific Meeting (IDSM 2017). Atlantis Press. Full text: https://www.researchgate.net/profile/Elza_Auerkari/publication/325729981_Molecular_Genetics_and_Epigenetics_of_Ankyloglossia/links/5b25d14a458515270fd41af9/Molecular-Genetics-and-Epigenetics-of-Ankyloglossia.pdf
- Øyen, N., Boyd, H. A., Poulsen, G., Wohlfahrt, J., & Melbye, M. (2009). Familial recurrence of midline birth defects—a nationwide danish cohort study. American journal of epidemiology, 170(1), 46-52. https://academic.oup.com/aje/article/170/1/46/134844


 What to Do About Keto Breath From a Low-Carb Diet
What to Do About Keto Breath From a Low-Carb Diet