Table of Contents[Hide][Show]
Cold sores, or “fever blisters”, are painful blisters that form on the face, usually near the lips.
They’re caused by one of the most common viral infections in the world. According to the CDC, nearly 50% of people have at least one cold sore outbreak every year.
You can’t cure cold sores permanently, but certain medications and home remedies may help shorten outbreaks and improve symptoms.
What is a cold sore?
A cold sore is a red or dark pink fluid-filled blister around the mouth caused by the herpes simplex virus. Cold sores may appear on other parts of your face. Rarely, cold sores can spread to your nose, inside of your mouth, or even your fingers.
Cold sores are also known as fever blisters, herpes labialis, or oral herpes.
Generally, cold sores spread through close contact, like kissing or oral sex, with another person during an outbreak. Even before you can see the blisters, cold sores may be contagious if skin contact is made.
Cold sores may come back at any time, even after an active outbreak has ended. There is no known cure for cold sores, which are a recurring skin condition.
Get Dr. B’s Dental Health Tips
You can’t be healthy without a healthy mouth. Sign up for my free newsletter and you’ll get my unconventional tips, starting with: If I had a cavity, here’s exactly what I’d do to reverse it.

What does a cold sore look like?
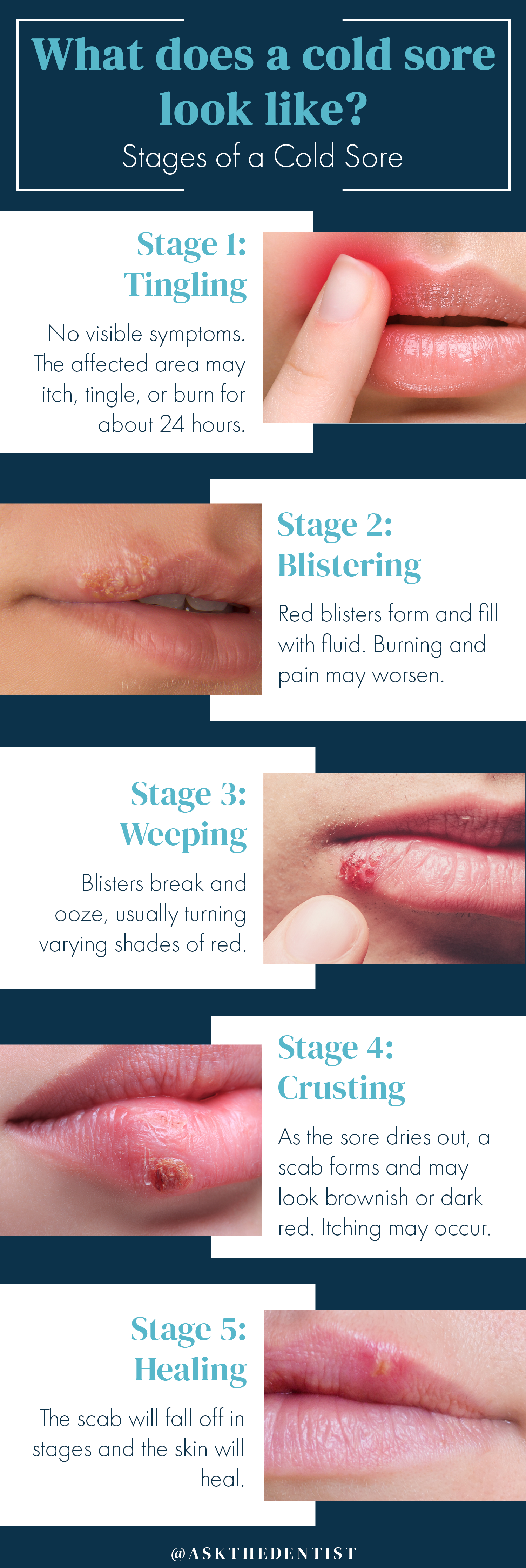
There are 5 cold sore stages that each look different:
- Stage 1/Tingling: For about 24 hours, your mouth may itch and/or tingle. Many people describe the feeling as a burning sensation. No visible signs may appear.
- Stage 2/Blistering: Blisters form and fill with fluid. You may develop several small blisters or one large blister. Sores appear white, greyish, or yellow while skin becomes inflamed and red.
- Stage 3/Weeping: Blisters break (burst) and may ooze. Painful sores form and are often varying shades of red.
- Stage 4/Crusting: After a few days, sores dry out and a scab forms. Itching and cracking are common.
- Stage 5/Healing: The scab falls off and the skin heals.
Cold sores are contagious at every stage until they heal completely. They spread most easily during stage 3.
You cannot speed up cold sore healing by popping it or by ripping off the scab. Both of these actions may lead to a scar once the cold sore has healed completely.
Cold Sore Symptoms
Tingling, burning, and itchy facial skin are the first signs of a fever blister/cold sore. Catching a cold sore early is important to shorten its duration, so begin treatment immediately.
As the cold sore virus progresses, you’ll experience pain and tenderness. Multiple sores may appear.
Especially during your first cold sore outbreak, you may also experience symptoms like:
- Sore throat
- Painful gums
- Dehydration
- Swollen lips
- Fever
- Headache
- Nausea
- Swelling of the lymph nodes
- General muscle and joint aches
During your first cold sore, you may contract gingivostomatitis, an infection of the gums and mouth. This may be accompanied by swollen lymph nodes, bad breath, and a desire to avoid drinking water.
Rarely, your eyes may become infected. If you experience any symptoms in or around your eyes during a cold sore infection, call a doctor immediately. HSV-1 infections in the eyes may lead to vision loss if not addressed right away.
What causes cold sores?
Cold sores are caused by the herpes simplex virus (HSV-1).
“Herpes” can sound alarming, but it’s an incredibly common virus. 50-80% of adults in the United States carry HSV-1, according to Johns Hopkins Medicine. However, some individuals never develop a cold sore even though they carry the virus.
Most people, however, will experience at least one or two cold sores in their lifetime.
The herpes virus “hides” in the ganglion of nerve cells under the skin of your face after an initial outbreak has ended. There, it is considered “dormant” or “latent.” When triggered again, HSV-1 replicates through the nerve and out to the skin to create a new cold sore. This is why recurring oral herpes outbreaks often happen around the same area of the face as prior outbreaks.
HSV-2 (herpes simplex virus 2) is a related viral strain that causes genital herpes. HSV-2 can rarely spread to the face, and HSV-1 can be transmitted to the genitals.
A person may not develop their first cold sore for up to 20 days after exposure to HSV-1. During this time, they may still spread the virus.
Risk Factors
As 90% of people carry the herpes virus that causes cold sores, most people are at risk of developing a cold sore at some point in their lifetime. A weak immune system is the most significant risk factor for cold sores.
If you have any of the following conditions, your immune system is weaker than average. This puts you at a higher risk of HSV-1 infections or complications:
- Eczema (atopic dermatitis)
- HIV/AIDS
- Autoimmune disease
- Third-degree burns over much of the body
- Cancer (especially during chemotherapy treatment)
- Organ transplants (because of anti-rejection drugs)
Certain genetic factors may also increase your risk of cold sores. The C21orf91 gene is associated with more frequent herpes labialis outbreaks.
What triggers a cold sore? New or recurring cold sore outbreaks may be triggered by:
- A weak immune system for any reason
- Any viral or bacterial infection (cold, flu, etc.)
- Sun exposure
- Chronic stress
- Fatigue
- Menstruation
- Dental work
- Injury to facial skin
Complications
In some cases, cold sore outbreaks may lead to serious medical complications such as:
- Eczema: Eczema combined with cold sore infections can cause eczema herpeticum, a potentially life-threatening medical emergency. People with eczema are more susceptible to cold sores because they have an inflammatory autoimmune condition across a large area of skin. No longer limited only to the face, cold sores can spread to any area of the body. This is most common in children.
- Herpetic whitlow: HSV-1 may be transferred to the fingertips, a condition known as herpetic whitlow (“whitlow finger”). This is why some babies and toddlers who suck their thumbs and fingers will get fever blisters on fingers. Dentists suffer from this type of cold sore complication more frequently than the general population.
- Eye infections: Herpes simplex can travel to the eyes and cause infections like herpetic keratoconjunctivitis or viral keratitis. This can result in inflammation and ulcers on the cornea. If left untreated, eye infections from cold sores can result in permanent vision loss. Call a doctor right away if you experience eye symptoms during a cold sore outbreak.
- Genital sores: Usually, HSV-1 causes cold sores on the face and HSV-2 causes genital herpes. However, it’s possible to spread HSV-1 sores to the genitals or HSV-2 sores to the face.
- Acute herpetic pharyngotonsillitis: In adults, cold sores may lead to this throat/tonsil infection. You may develop a fever, headache, tiredness, and a sore throat, but this infection is not usually serious.
- Gingivostomatitis: This gum/mouth infection usually happens only once, if ever, and heals in 7-10 days. However, it can spread to the central nervous system and may lead to meningoencephalitis and/or death.
- Meningitis or encephalitis: In immunocompromised individuals, HSV viruses may travel to and cause inflammation in the spinal cord (meningitis) and brain (encephalitis). This is a very rare and dangerous complication of the herpes virus.
When to Call a Doctor
Most cold sores can be treated at home without problems. However, children and people at risk of complications should be monitored more closely and may need professional attention.
You should contact a doctor immediately if you or your child have a cold sore and:
- High or long-lasting fever
- Breathing or swallowing problems
- Irritation around the eyes which may or may not cause redness or discharge
- The spread of cold sores to an eczema breakout
You should also call your doctor if you develop a cold sore and have a compromised immune system, such as with cancer or AIDS.
Diagnosis
To diagnose a cold sore, your doctor can perform a physical exam. Cold sores are usually easy to identify, but he or she may order lab tests to confirm the diagnosis in some cases.
If you are at high risk of complications, your physician may sample the fluid from an oozing cold sore.
Cold Sore Treatment
How do you get rid of a cold sore fast? Over-the-counter topical ointments or creams like Abreva may shorten the length of a cold sore outbreak.
In some cases, your doctor may recommend prescription antiviral medications to prevent recurring infections.
Several home remedies may also improve symptoms of cold sores.
According to available scientific evidence, no treatment can get rid of a cold sore in 24 hours.
Without treatment, most cold sore infections will clear up within 7-10 days.
Creams & Ointments
Prescription topical creams or ointments that your doctor may prescribe for a cold sore include:
- Viroxyn Professional (benzalkonium chloride and benzocaine)
- Xerese (acyclovir and hydrocortisone)
- Soothelip (acyclovir)
- Denavir (penciclovir)
Viroxyn may be able to reduce the time to cold sore healing by over 3 days more than Abreva. A 2010 study found Viroxyn healed a cold sore in just 4 days on average.
Over-the-counter topical creams or ointments that may help improve cold sore symptoms and/or shorten an outbreak include:
- Abreva (docosanol)
- Zinc oxide cream (typically sold for diaper rash)
- Aloe vera gel
- Zilactin (benzyl alcohol)
Abreva (docosanol) is the only over-the-counter antiviral treatment approved by the FDA to shorten the healing time of cold sores. Abreva may heal a cold sore in just 4-7 days.
Aloe vera gel and zinc oxide cream may also shorten outbreaks and reduce cold sore symptoms.
Zilactin is marketed for topical cold sore relief. No studies support its efficacy for improving symptoms, but it may dry out the area and reduce the pain caused by a cold sore.
All topical creams or gels for cold sores should be applied to the tingling or burning area 4-5 times each day for maximum effectiveness.
Touching a cold sore directly greatly increases your risk of spreading the infection to another part of your body or another person. When using creams and ointments for cold sores, always apply with a cotton swab.
Medications
Oral medications are available by prescription for prolonged or recurring cold sore infections:
- Zovirax (acyclovir)
- Valtrex (valacyclovir)
- Famvir (famciclovir)
These antiviral medicines may be prescribed for daily use if you have frequent cold sore outbreaks and/or you are at a high risk of complications.
Home Remedies
Several cold sore remedies may improve your symptoms or even reduce your risk of future infections. These include:
- Bee propolis
- Apple cider vinegar
- Essential oils (eucalyptus, tea tree, peppermint, ginger, thyme, hyssop, and sandalwood)
- Lemon balm (salve or oral dietary supplement)
- Kanuka honey
- Aloe vera gel
- Lysine
Does toothpaste get rid of cold sores? No one knows for sure if toothpaste can get rid of cold sores. Anecdotal reports suggest that toothpaste containing SLS may help to dry out cold sores. However, no scientific evidence supports this claim.
Sodium lauryl sulfate (SLS) may actually cause canker sores, so avoid using this as a treatment for your cold sores.
Cold Sore Pain Relief
Even if your infection time is shortened by effective treatment, you’ll probably still experience pain during your outbreak.
To reduce pain from a cold sore:
- Use ice or a cold compress against the skin
- Take over-the-counter painkillers like ibuprofen (Advil) or acetaminophen (Tylenol)
- Use benzocaine or lidocaine gel to numb the area
Remember not to touch the sore with your hands and use a cotton ball or swab when applying a topical anesthetic.
Aspirin should not be used for cold sore pain — or any pain during a viral infection — especially in children.
Rarely, aspirin use during a viral infection may lead to Reye syndrome, a serious childhood condition that begins with persistent vomiting and may lead to neurological problems and other life-threatening complications.
How to Prevent Cold Sores
The virus is generally passed through skin contact or by touching personal items used by an infected person. To prevent spreading cold sores, do not:
- Share drinking glasses, water bottles, or eating utensils
- Use someone else’s lip balm
- Share toothbrushes or other hygiene products
- Kiss someone who has a cold sore or has been in close contact with another person who has a cold sore
- Perform or receive oral sex with someone who may have a cold sore or genital herpes
You should also wash your hands frequently and thoroughly during a cold sore outbreak.
To prevent or reduce your risk for recurring cold sore infections, you should avoid triggers for new outbreaks and keep your immune system healthy:
- Use a lip balm with sunscreen: Use an SPF 30 or higher lip balm.
- Avoid sun overexposure: Always use sunscreen and avoid spending several hours in the sun on a regular basis.
- Replace your toothbrush regularly: Your toothbrush or toothbrush head can hang onto viruses including HSV-1. Replace your toothbrush every 1-3 months and immediately after a cold sore outbreak.
- Practice stress-relief techniques: Journaling, meditation, time outdoors, exercise, and restful sleep can all help reduce stress and fatigue that can trigger cold sores.
- Support immune health during menstruation: Women may be more prone to cold sores during their periods. Don’t neglect immunity and healthy habits/eating during your cycle, as this could increase your risk of new cold sores.
- Boost your immune system: As with any virus, cold sores are less likely if your immune system is strong. Ensure you’re getting plenty of vitamin C, vitamin D, and nutrient-dense foods. You may also try a probiotic supplement and/or oral probiotics to support a healthy microbiome.
- Be cautious after dental work: Dental cleanings and other procedures can temporarily weaken your immune system by exposing your bloodstream to higher amounts of oral bacteria than normal.
How long do cold sores last?
First cold sore outbreaks may last as long as 2 weeks.
Recurrent outbreaks usually heal in 7-10 days.
The cold sore virus does not go away, even when a cold sore outbreak has healed. It remains dormant in nerve cells until the infection is triggered again.
Cold Sores vs. Canker Sores
A cold sore outbreak is the result of a viral infection, while canker sores are non-contagious ulcers caused by several different factors.
The easiest way to spot the difference between cold sores and canker sores is by their location and appearance.
| Cold Sore | Canker Sore | |
|---|---|---|
| Location | Face, usually on or around the lips | Inside the mouth, on the tongue, cheeks, or throat |
| Appearance | Raised, red, fluid-filled blisters; eventually, ooze then scab over | Flat, red circular ulcers surrounded by a white halo |
| Causes | Viral infection from herpes simplex virus 1 (HSV-1) Outbreaks may be triggered by: – Weakened immunity – Stress – Sun exposure – Hormonal imbalance | – Injury (biting your cheek) – Toothpaste with sodium lauryl sulfate (SLS) – Zinc, iron, or vitamin B12 deficiency – Hormonal imbalance – Oral microbiome imbalance |
| Time to Recovery | 7-14 days | 1-6 weeks |
| Contagious? | Yes | No |
Popping a Cold Sore
Does popping a cold sore help it heal faster? No, popping a cold sore does not help the blister heal faster. In fact, popping your cold sore will more than likely lead to:
- More cold sores as the blister fluid spreads
- Risk of new, different infections by exposing an open sore
- Scarring
- Increased pain
Popping a cold sore is especially dangerous if you are at risk of complications due to a compromised immune system. Skin conditions like eczema or psoriasis make it easier for the HSV-1 virus to spread all over the body, which may lead to life-threatening complications.
FAQs
Are there clinical trials available for people with frequent cold sores?
The US National Library of Medicine has a database for active clinical trials for oral herpes treatments.
Do cold sores mean you have an STD?
Most people contract the HSV-1 virus during childhood years, not related to any type of sexual contact. Cold sores are not considered an STD, unlike genital herpes caused by HSV-2.
Keep in mind, though, that HSV-2 outbreaks in the genital area can pass to the mouth during oral sex and cause sores on the face. It’s also harder to prevent with condoms than other STDs since it can be transferred from the skin not covered by a condom.If you’re concerned you’ve contracted the HSV-2 virus, see your doctor for treatment options.
Cold Sores vs. Canker Sores: Why You Should Know the Difference
References
- McQuillan, G. M., Kruszon-Moran, D., Flagg, E. W., & Paulose-Ram, R. (2018). Prevalence of herpes simplex virus type 1 and type 2 in persons aged 14-49: United States, 2015-2016 (pp. 1-8). US Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Health Statistics. Full text: https://www.cdc.gov/nchs/products/databriefs/db304.htm
- Kolokotronis, A., & Doumas, S. (2006). Herpes simplex virus infection, with particular reference to the progression and complications of primary herpetic gingivostomatitis. Clinical microbiology and infection, 12(3), 202-211. Full text: https://www.researchgate.net/profile/Stergios_Doumas/publication/7323444_Herpes_simplex_virus_infection_with_particular_reference_to_the_progression_and_complications_of_primary_herpetic_gingivostomatitis/links/59dd40ba458515f6efef4cd7/Herpes-simplex-virus-infection-with-particular-reference-to-the-progression-and-complications-of-primary-herpetic-gingivostomatitis.pdf
- Arduino, P. G., & Porter, S. R. (2008). Herpes Simplex Virus Type 1 infection: overview on relevant clinico‐pathological features. Journal of oral pathology & medicine, 37(2), 107-121. Abstract: https://www.ncbi.nlm.nih.gov/pubmed/18197856
- Kriesel, J. D., Jones, B. B., Matsunami, N., Patel, M. K., St. Pierre, C. A., Kurt-Jones, E. A., … & Hobbs, M. R. (2011). C21orf91 genotypes correlate with herpes simplex labialis (cold sore) frequency: description of a cold sore susceptibility gene. Journal of Infectious Diseases, 204(11), 1654-1662. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3203230/
- Rowe, N. H., Heine, C. S., & Kowalski, C. J. (1982). Herpetic whitlow: an occupational disease of practicing dentists. Journal of the American Dental Association (1939), 105(3), 471-473. Abstract: https://www.ncbi.nlm.nih.gov/pubmed/6957456
- Dawson, C. R., & Togni, B. (1976). Herpes simplex eye infections: clinical manifestations, pathogenesis and management. Survey of ophthalmology, 21(2), 121-135. Abstract: https://www.ncbi.nlm.nih.gov/pubmed/988644
- Klastersky, J., Cappel, R., Snoeck, J. M., Flament, J., & Thiry, L. (1972). Ascending myelitis in association with herpes-simplex virus. New England Journal of Medicine, 287(4), 182-184. Abstract: https://www.nejm.org/doi/pdf/10.1056/NEJM197207272870411
- Mccarthy, J. P., Browning, W. D., Teerlink, C., & Veit, G. (2012). Treatment of herpes labialis: comparison of two OTC drugs and untreated controls. Journal of Esthetic and Restorative Dentistry, 24(2), 103-109. Full text: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3472024/
- Sacks, S. L., Thisted, R. A., Jones, T. M., Barbarash, R. A., Mikolich, D. J., Ruoff, G. E., … & Morrow, P. R. (2001). Clinical efficacy of topical docosanol 10% cream for herpes simplex labialis: a multicenter, randomized, placebo-controlled trial. Journal of the American Academy of Dermatology, 45(2), 222-230. Abstract: https://pubmed.ncbi.nlm.nih.gov/11464183/
- Godfrey, H. R., Godfrey, N. J., Godfrey, J. C., & Riley, D. (2001). A randomized clinical trial on the treatment of oral herpes with topical zinc oxide/glycine. Alternative therapies in health and medicine, 7(3), 49. Abstract: https://pubmed.ncbi.nlm.nih.gov/11347285/
- Rezazadeh, F., Moshaverinia, M., Motamedifar, M., & Alyaseri, M. (2016). Assessment of anti HSV-1 activity of Aloe vera gel extract: an in vitro study. Journal of Dentistry, 17(1), 49. Abstract: https://pubmed.ncbi.nlm.nih.gov/26966709/
- Chavan, M., Jain, H., Diwan, N., Khedkar, S., Shete, A., & Durkar, S. (2012). Recurrent aphthous stomatitis: a review. Journal of Oral Pathology & Medicine, 41(8), 577-583. Full text: https://www.researchgate.net/profile/Mahesh_Chavan5/publication/221891773_Recurrent_aphthous_stomatitis_A_review/links/5b69611392851ca650512153/Recurrent-aphthous-stomatitis-A-review.pdf

 Dental Sealants: What are they, are they safe, and do they work?
Dental Sealants: What are they, are they safe, and do they work?