Table of Contents[Hide][Show]
I have a 2 year old daughter. I have been brushing her teeth with childrens' toothpaste for 1 year. On the back of the childrens' toothpaste it says it contains 500ppm fluoride. She has been eating this stuff for a year because she can't spit. I feel horrible. Now she has what looks to be mild fluorosis. We switched to non-fluoride toothpaste but I am concerned that her permanent teeth have already been affected. Will she have fluorosis on those too?
First, make sure it is fluorosis you are dealing with. Deficiencies of other nutrients like calcium, phosphorus, and vitamin D can lead to something that looks like fluorosis.
There are other dental diseases like amelogenesis imperfecta that can sometimes look like motteled teeth. Sometimes brownish or whitish spots can occur if there are bottle-feeding cavities. Your dentist will be able to identify it. In the meantime, I recommend using a non-fluoride toothpaste up until age 10.
Although fluorosis is an irreversible condition, it can be ameliorated with cosmetic dentistry during the early adult years. But this is an expensive solution that does not last. In moderate to severe fluorosis, the cavity and decay rate is greatly increased. This means that your daughter will need many dental visits for fillings at a formative age and this must be done with great care as not to create a fearful patient later in adulthood.
Fluorosis: What It Is and How to Prevent It
Any amount of fluoride can cause fluorosis. Fluorosis is a condition caused by too much fluoride during the years that a tooth develops inside the jawbone. It causes aesthetic and structural defects in the tooth. It can be caused by swallowing toothpaste with fluoride in it, consuming too much fluoride (via drinking water) or too many fluoride supplements (such as fluoride tablets) given by parents or pediatricians.
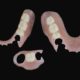
Examples of varying stages of fluorosis:
https://www.instagram.com/p/B65loQnpo-R/?utm_source=ig_embed&utm_medium=loading
https://www.instagram.com/p/B9ZYGEBg79Q/?utm_source=ig_embed&utm_medium=loading
Ideally, when your child first shows signs of teeth erupting, you should contact your dentist and ask about the appropriate amount of fluoride for your child. Your dentist should know what the local fluoride concentrations is in the water supply and can make you a recommendation based on that. That includes advice on drinking water from the tap, advice on other drinks like tea or bottled water. If you do give your child fluoride, it is mandatory that you and your dentist know exactly how much your child is ingesting up intil age 10.
I have seen fluorosis even without purposeful ingestion of fluoride. Many of my patients from the southwest seem to have higher rates of mottled teeth, probably due to ground water or well water with high mineral contents.
Get Dr. B’s Dental Health Tips
Free weekly dental health advice in your inbox, plus 10 Insider Secrets to Dental Care as a free download when you sign up

Fluoride Isn’t Only In Water
Formula fed infants receive 50 to 100 times more fluoride than exclusively breast fed infants. Fluoride can even be ingested by breathing in certain contaminants in the air.
Fluoride can be transferred from the mother to the fetus through the placenta. Fluoride is inhaled, ingested, absorbed by the body, then goes into the the blood stream, then deposited into the bones.
Previous fluoride exposures can determine the current ratio of ingestion to excretion. The balance of fluoride in the body is very complex and is difficult to quantify.
It is such a complicated and poorly measured process that it scares me to think that we think we know the optimal amount of fluoride that we have to add to our children’s drinking water and diet.
Sources of Fluoride: It’s (Almost) Everywhere
- Toothpaste
- Tap water
- Infant Formula
- Processed cereals
- Juice
- Soda
- Tea
- Wine
- Beer
- Mechanically de-boned chicken
- Fish and seafood
- Teflon pans
- Fluoridated salt
- Inhalation anaesthetics
- Cigarettes
- Second-hand smoke
- Pesticides
I recommend keeping track of where your child is getting fluoride from, and how much.
The dose is greater for children than it is to adults based on the mg/kg body weight formula for fluoride consumption. In other words, if you are a little person, your exposure to and the potential effects of fluoride are greater.
Fluorosis In Children Is on the Rise
Parents and even dentists are confused as to how much fluoride there is taken in and where it’s all coming from.
The amounts that could potentially be ingested by our children and by ourselves need to be carefully quantified. We need to know the fluoride concentration of our drinking water.
We need to supervise the use of toothpaste in children under six. Parents need consult a dentist before brushing their child’s teeth and before toothpaste is used.
Only a pea-sized amount can be used. Keep the toothpaste out of reach.
Find a different water source for children eight years of age or younger whose primary drinking water contains greater than 2 ppm fluoride (common in some regions in the US) as this will put them at an increased risk of fluorosis.
References
From the Center for Disease Control and Prevention:
“A nine percentage point increase in the prevalence of very mild or greater fluorosis was observed among children and adolescents aged 6-19 years when data from 1999-2002 were compared with those from the NIDR 1986-1987 survey of school children (from 22.8% in 1986-1987 to 32% in 1999-2002).”
SOURCE: Centers for Disease Control and Prevention (CDC, 2005) Surveillance for dental caries, dental sealants, tooth retention, edentulism, and enamel fluorosis–United States, 1988-1994 and 1999-2002. Morbidity and Mortality Weekly Report Surveillance Summaries 54:1-43.
“The prevalence of fluorosis in permanent teeth in areas with fluoridated water has increased from about 10-15% in the 1940s to as high as 70% in recent studies…”
SOURCE: Marshall TA, et al. (2004). Associations between Intakes of Fluoride from Beverages during Infancy and Dental Fluorosis of Primary Teeth. Journal of the American College of Nutrition 23:108-16.
“There is compelling evidence that the prevalence of dental fluorosis has increased in the United States and Canada in recent years.”
SOURCE: Warren JJ, Levy SM. (2003). Current and future role of fluoride in nutrition. Dental Clinics of North America 47: 225-43.

 What are Receding Gums? How to Prevent and Treat Gum Recession
What are Receding Gums? How to Prevent and Treat Gum Recession